Translate this page into:
Human leukocyte antigen in patients with psoriasis
2 Division of Immunopathology, Department of Dermatology and Venereology, Institute of Medical Sciences, Varanasi, Uttar Pradesh, India
Correspondence Address:
Sangeeta Singh
Division of Immunopathology, Department of Pathology, Institute of Medical Sciences, Banaras Hindu University, Varanasi - 221 005, Uttar Pradesh
India
| How to cite this article: Singh S, Singh U, Singh S. Human leukocyte antigen in patients with psoriasis. Indian J Dermatol Venereol Leprol 2011;77:535 |
Sir,
Psoriasis is a common skin disease. Various studies all over the world support the association of HLA antigens with psoriasis. [1] It is a multifactorial and heterogenetically inherited disease. Genetic background of psoriasis is supported by familial association, twin studies, and correlation with human leukocyte antigens. [2] The present study was done to see the expression of HLA- A, B, C, DR, and DQ antigens in patients with psoriasis.
Seventy-five patients (46 males, 29 females; mean age 38.2±16.3 years) presenting to the outpatient Department of Dermatology and Venereology, SS Hospital, BHU, Varanasi and 75 controls (42 males, 33 females; 35.7±11.6 years) were included. Fifty-four (72%) patients had early onset of disease while 21 (28%) patients had late onset of disease. Controls were the volunteers from the staff and student of the Institute of Medical Sciences without any present or past history of autoimmune disease, systemic disease, and skin disorder. Typing for HLA- A, B, C, DR, and DQ antigens was performed by the microcytotoxicity method. [3] Antisera used for HLA typing were of BAG Health care GmbH, Lich, Germany. Informed consent was taken from all patients and controls and the study was approved by the ethical committee of the institution. Statistical analysis was done using SPSS 14.0 (SPSS Inc., Chicago, IL, USA). Pearson′s χ2 with Yates′ correction for continuity was performed to analyze the significance of each HLA antigens in patients with psoriasis versus controls. Fisher′s exact test was performed if expected frequency of an antigen was less than 5.
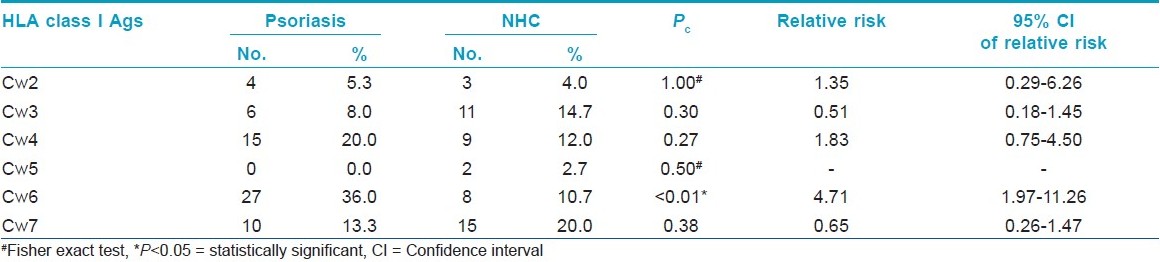
Among HLA-A antigen group A1, A24 and A28 were significantly increased in psoriasis patients as compared to control. The frequency of HLA-A3 was more in control as compared to psoriasis patients (14.7% vs 6.7%) while HLA-A24 and A26 were not expressed in control [Table - 1]. In HLA-B group, B13 was not detected in the psoriasis group, while it was detected in 9.3% control cases. HLA-B17 and B35 were more frequently detected in psoriasis patients than in control group but it was not significant [Table - 2]. Among HLA-C group only Cw6 was significantly increased in the psoriasis group as compared to control (36.0% vs 10.7%, P<0.01) [Table - 3]. In HLA-DR and DQ group, HLA-DR3 was significantly elevated in psoriasis patients, while in control it was not detected. HLA- DR53 was also significantly elevated as compared to control. DQ1 was significantly elevated in psoriasis as compared to control [Table - 4].
Psoriasis develops by the interaction of genetic, immunological, and environmental factors. Previous studies have reported a significant association of HLA class I and II antigens in patients with psoriasis which suggests the genetic background of psoriasis and role of HLA in its pathogenesis. Ray et al. [4] had done HLA typing of patients with psoriatic arthritis in India and found a significant association with HLA- A1, B17. In our study, we also found a significant association with HLA- A1, while HLA- B17 was found in high frequency in patients with psoriasis but it was insignificant. A study on Croation patients reported a significant association of HLA- B13, B17, Cw6, and DR7 antigens in patients of psoriasis. [5] Contrary to these above studies we did not find any positive correlation with HLA- B13, in fact B13 was not detected in patients. It was seen only in control. We also found slightly increased but insignificant frequency of B17 (19.5% vs 11.1%) and DR7 (50.6% vs 40.2%) in psoriasis patients as compared to controls. Our study showed a significant increase in the HLA-Cw6 antigen in patients with psoriasis. Various studies on patients with psoriasis have also shown strong association with HLA- Cw6 in patients with psoriasis. The HLA- Cw6 antigen was significantly expressed in our patient with a relative risk of 5.18.
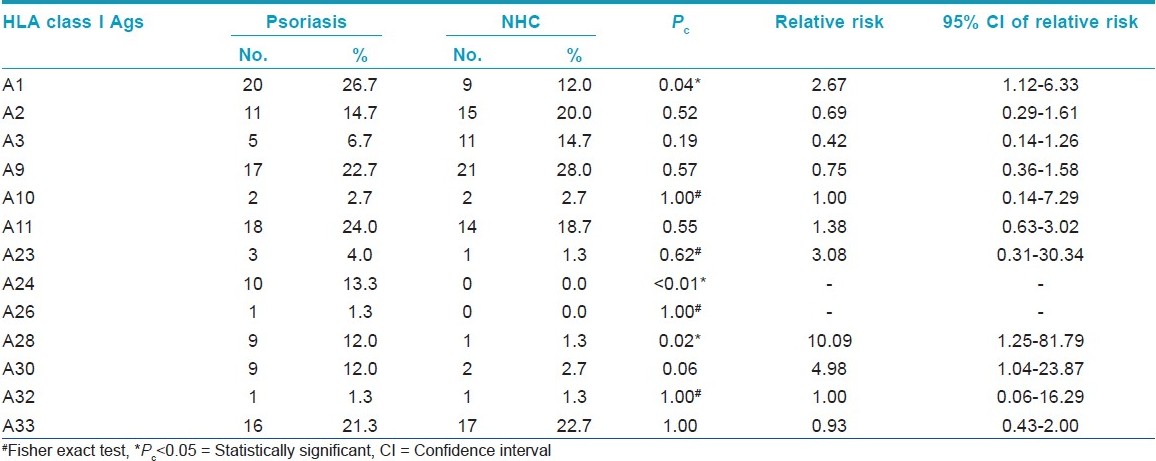

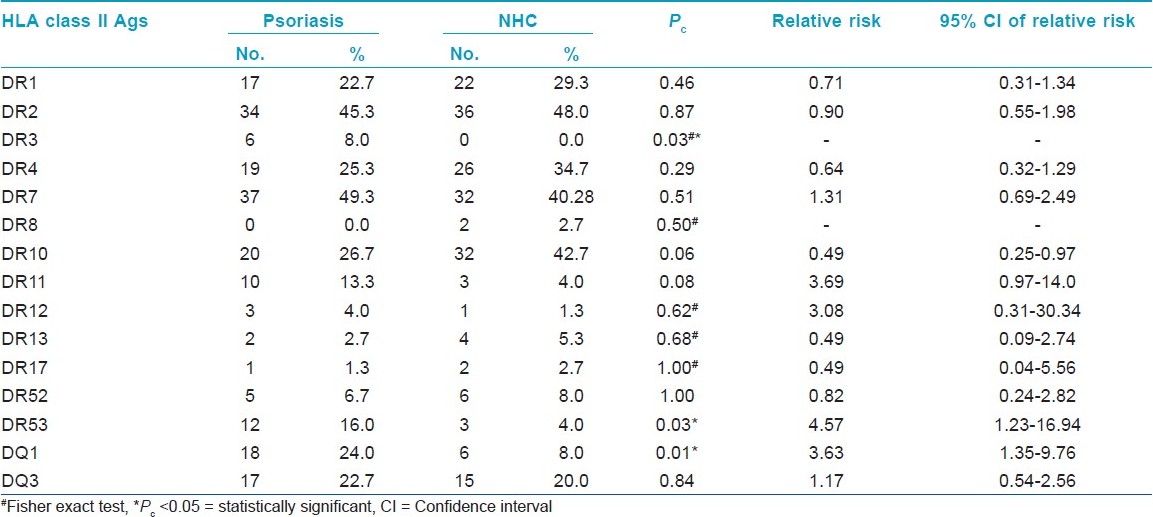
HLA- A33 (21.3% vs 22.7%, RR 0.93), B7 (12.0% vs 10.7%, RR 1.00), B12 (13.3% vs 13.3%, RR 1.00), Bw4 (25.3% vs 22.7%, RR 1.16), Bw6 (57.3% vs 56.0%, RR 1.0), and DR2 (45.3% vs 48.0% RR 0.90) were expressed at same frequency in patients as well as controls. Thus our study concludes that HLA- A1, A24, A28, A30, B35, Cw6, DR3, and DQ1 are more common in patients with psoriasis in our study group. These antigens may be involved in pathogenesis of psoriasis in our region.
| 1. |
Henseler T. The genetics of psoriasis. J Am Acad Dermatol 1997;37:S1-11.
[Google Scholar]
|
| 2. |
Szczerkowska-Dobosz A, Rebala K, Szczerkowska Z, Witkowska-Tobola A. Correlation of HLA-Cw*06 allele frequency with some clinical features of psoriasis vulgaris in the population of northern Poland. J Appl Genet 2004;45:473-6.
[Google Scholar]
|
| 3. |
Terasaki PI, McClelland JD. Microdroplet assay of human serum cytotoxins. Nature 1964;204:998-1000.
[Google Scholar]
|
| 4. |
Ray SC, Singh T, Kaur I, Suri S, Sehgal S, Kaur S. Clinical profile of psoriatic arthropathy. Indian J Dermatol Venereol Leprol 1990;56:200-3.
[Google Scholar]
|
| 5. |
Kastelan M, Gruber F, Cecuk E, Kerhin-Brkljacic V, Brkljacic-Surkalovic L, Kastelan A. Analysis of HLA antigens in Croatian patients with psoriasis. Acta Derm Venereol Suppl (Stockh) 2000;211:12-3.
[Google Scholar]
|
Fulltext Views
1,401
PDF downloads
1,239





