Translate this page into:
Isolated oral mucosal leishmaniasis
2 Department of Microbiology, Aditya Birla Sankar Nethralaya Laboratory Services, Kolkata, India
3 Department of Microbiology, All India Institute of Medical Sciences, New Delhi, India
4 Department of Dermatology, Dr. Ram Manohar Lohia Hospital, New Delhi, India
Correspondence Address:
Jyotish Chander Samantaray
Department of Microbiology, All India Institute of Medical Sciences, New Delhi - 110 029
India
| How to cite this article: Ahmed NH, Mukherjee A, Samantaray JC, Kar HK. Isolated oral mucosal leishmaniasis. Indian J Dermatol Venereol Leprol 2014;80:343-345 |
Sir,
A 34-year-old man from Bihar, which is a state endemic for kala-azar in India, had a one-and a half year history of a fleshy swelling inside the oral cavity accompanied by a change in his voice and difficulty in deglutition. The swelling began as an approximately 1 cm sized nodule on the hard palate that increased progressively in size. The patient was not a smoker or alcoholic and was not promiscuous. He gave no history of any surgery, blood transfusions or drug abuse.
A biopsy had been taken from the mass and the report stated that there were numerous ill-formed granulomas with overall features of chronic inflammation without significant atypia. Based on the biopsy report, the patient was prescribed anti-tubercular treatment (ATT) by his physicians. The patient was referred to New Delhi when no improvement was noted after two months of treatment.
On examination, a proliferative fleshy growth with a cauliflower-like surface was noted within the buccal cavity involving the entire hard and soft palate and both the tonsils and extending to the posterior pharyngeal wall [Figure - 1]. The lesion was confined to the oral cavity. There were no skin lesions. The jugulo-digastric lymph nodes on both sides and multiple lymph nodes in the posterior triangle were enlarged. Routine laboratory tests were within normal limits. Contrast enhanced CT scan of the neck showed a homogeneous, lobulated, strongly enhancing mass lesion involving the hard and soft palate and extending into the nasopharyngeal air column. A soft tissue mass was also seen at the posterior end of the nasal septum and within the right nostril. A dense, lobulated, soft tissue mass filling up the right pyriform fossa, pharyngeal mucosal spaces, vallecula and also pre- and para-laryngeal fat spaces was noted.
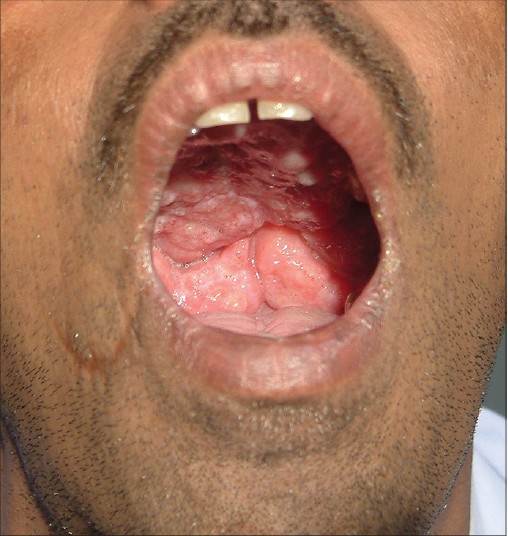 |
| Figure 1: Before treatment, proliferative growth in the buccal cavity involving the hard palate, soft palate, tonsils and posterior pharyngeal wall |
A repeat biopsy was taken from the mucosal mass. Impression smears from the biopsy were sent for parasitological workup to the Microbiology department, All India Institute of Medical Sciences, New Delhi. Giemsa and acridine-orange stained smears revealed numerous Leishman-Donovan (LD) bodies. The serum aldehyde test was positive and serum total protein was 8.7 g%, with albumin being 3.9 g% and globulin 4.8 g%. The test for serum antibodies against L. donovani-specific kinesin antigen (rK-39) was positive by an immune-chromatography test (InBios International, Washington 98104, USA).
A diagnosis of mucosal leishmaniasis caused by L. donovani was made and the patient was subsequently treated with intramuscular sodium stibogluconate 800 mg daily for 20 days. There was prompt improvement with clearance of the larynx and disappearance of the growth [Figure - 2]. At follow up, microscopy of a biopsy from fibrotic remnants of the lesion was negative for LD bodies and histopathological examination revealed fibrotic and mild inflammatory changes. The serum rK-39 antibody test, however, continued to remain weakly positive.
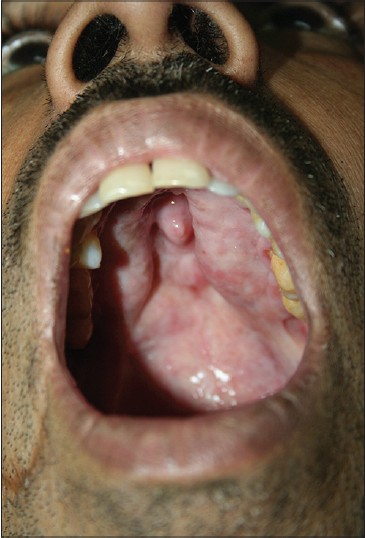 |
| Figure 2: After treatment, complete regression of the mass barring the small fi brotic remnant persisting in the hard palate |
Visceral leishmaniasis is endemic in some states of India; small outbreaks of cutaneous leishmaniasis due to L. donovani were also reported from India and Sri Lanka but mucosal leishmaniasis is exceedingly rare in the subcontinent. [1]
Mucosal leishmaniasis is most commonly associated with Leishmania braziliensis, and is limited mostly to South America. There are rare reports of mucosal involvement by L. donovani in Sudan. [2] Mucosal leishmaniasis does not heal spontaneously; secondary bacterial infections and other complications are common making the disease potentially fatal.
In the presence of immune deficiency/suppression, L. donovani can manifest in an unusual manner but in an immunocompetent person, leishmaniasis presenting as an isolated mucosal lesion without any cutaneous manifestations is exceedingly rare. [3],[4],[5],[6] Naik et al. in 1978, reported a case of leishmaniasis in which a huge nasopharyngeal tumor was the presenting complaint; however, a final diagnosis of visceral leishmaniasis was made because of accompanying systemic manifestations and demonstration of LD bodies in the splenic aspirate. [7] Cases with atypical clinical manifestations can be initially missed as happened in the present case. Specific diagnosis followed by appropriate treatment eventually resulted in cure of the disease. A high index of clinical suspicion for leishmaniasis is warranted in patients coming from endemic areas.
| 1. |
Sharma NL, Mahajan VK, Kanga A, Sood A, Katoch VM, Mauricio I, et al. Localized cutaneous leishmaniasis due to leishmania donovani and leishmania tropica: Preliminary findings of the study of 161 new cases from a new endemic focus in Himachal Pradesh, India. Am J Trop Med Hyg 2005;72:819-24.
[Google Scholar]
|
| 2. |
Mahdi M, Elamin EM, Melville SE, Musa MA, Blackwell JM, Mukhtar MM, et al. Sudanese mucosal leishmaniasis: Isolation of a parasite within the Leishmania donovani complex that differs genotypically from L. donovani causing classical visceral leishmaniasis. Infect Genet Evol 2005;5:29-33
[Google Scholar]
|
| 3. |
Singh S. Mucosal leishmaniasis in an Indian AIDS patient. Lancet Infect Dis 2004;4:660-1.
[Google Scholar]
|
| 4. |
Rathnayake D, Ranawake RR, Sirimanna G, Siriwardhane Y, Karunaweera N, De Silva R. Co-infection of mucosal leishmaniasis and extra pulmonary tuberculosis in a patient with inherent immune deficiency. Int J Dermatol 2010;49:549-51.
[Google Scholar]
|
| 5. |
Mathur SR, Ray R, Handa KK. Isolated laryngeal leishmaniasis in an immunocompetent patient in India. Trop Doct 2006;36:55-6.
[Google Scholar]
|
| 6. |
Sethuraman G, Sharma VK, Salotra P. Indian mucosal leishmaniasis due to Leishmania donovani infection. N Engl J Med 2008;358:313-5.
[Google Scholar]
|
| 7. |
Naik SR, Vinayak VK, Talwar P, Sehgal S, Mehra YN, Dutta BN, et al. Visceral leishmaniasis masquerading as a nasopharyngeal tumour. Report of a case. Trans R Soc Trop Med Hyg 1978;72:43-5.
[Google Scholar]
|
Fulltext Views
1,931
PDF downloads
907





