Translate this page into:
Lingua villosa nigra in an infant
Corresponding author: Dr. Shibhani Sudheer Hegde, Department of Dermatology, Bharati Vidyapeeth Medical College and Hospital, Katraj, Pune, India. shibhani.s.hegde@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Shah S, Hegde SS. Lingua villosa nigra in an infant. Indian J Dermatol Venereol Leprol. 2024;90:804-6. doi: 10.25259/IJDVL_1145_2023
Dear Editor,
Black hairy tongue (BHT) or lingua villosa nigra is an acquired, asymptomatic, benign and self-limiting condition rarely seen in infancy.1 It gets its name due to the hypertrophic reaction of keratin seen in filiform papillae giving it a black hairy appearance. This condition is commonly seen in adults above the age of 40 years and is uncommon in infancy.
Here, we report the case of an infant with BHT and discuss the various differential diagnoses of pigmentation in the oral cavity. A 6-month-old male child was brought by worried parents to the dermatology outpatients with complaints of sudden blackish discolouration of the tongue that was noticed a week ago. No prior history of intake of antibiotics or any other medication was reported. The child was still exclusively breastfed and the mother reported no change in the feeding habits and no feeding difficulties since the onset of the lesion. The infant’s birth history was unremarkable. No family history of Addison’s disease was reported. The child was otherwise normal with no other muco-cutaneous findings.
On examination, there was diffuse black discolouration of the dorsum of the tongue sparing the tip and lateral borders [Figure 1]. The scraping from the tongue revealed only epithelial cells and a few bacteria. A diagnosis of BHT was made. Parents were reassured regarding the benign and self-resolving nature of this condition. On follow-up after 4 weeks, there was complete clearance of the pigmentation.
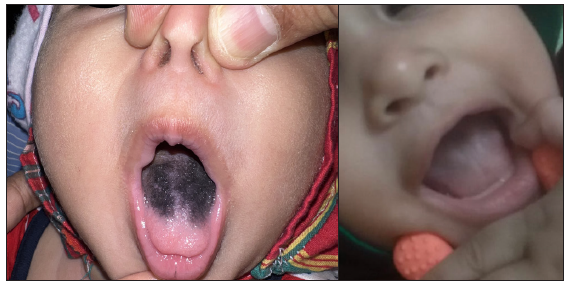
- Black discolouration of the dorsal surface of the tongue in a 6-month-old infant.
BHT (Syn; lingua villosa nigra, keratomycosis linguae, verbatum2 lingua or hyperkeratosis of the tongue) is a well-described and common pigmentary disorder of the tongue.2 Delayed desquamation and retention of papillary cells result in build-up of keratin which contributes to the hairy appearance of the tongue, with the length of the papillae reaching more than three times the normal length of the filiform papillae.3 Other than the black discoloration, the elongated papillae may appear brown, green or yellow in colour or may be devoid of any pigmentation. This retention leads to further changes in the oral environment leading to an increase in porphyrin-producing bacteria giving the characteristic black colour. However, other colours are not explained through the bacterial overgrowth and BHT is not considered a true infectious glossitis.4,5
The aetiology of BHT is not fully elucidated and is multifactorial. Various local and systemic insults contribute to an altered oral pH and promotion of chromogenic bacteria. A typical patient of BHT would be an older male smoker with a blackish coating on the tongue and complaints of dysgeusia, halitosis or a burning sensation in the mouth.2 Infants presenting with BHT vary significantly from their adult counterparts [Table 1].2,5 Epidemiological data regarding infantile BHT is scarce. All prior prevalence data is exclusive to adult BHT.5 Differential diagnoses to be considered during infancy are congenital melanocytic naevus, pseudo BHT (chemical- or food colouring–induced discolouration), lingual melanotic macules, Addison’s disease, pigmented fungiform papillae of the tongue and Peutz-Jeghers syndrome. Differential diagnoses and their classical features are mentioned in Table 2.2,3,5-7
| Features | Adult black hairy tongue | Infantile black hairy tongue |
|---|---|---|
|
|
|
| Symptoms |
|
|
| Course |
|
|
| Risk factors |
|
|
| Differential diagnosis |
|
|
| Treatment |
|
|
| Condition | Classical features |
|---|---|
| Black hairy tongue |
|
| Pseudo hairy tongue |
|
| Pigmented fungiform papillae of the tongue |
|
| Congenital melanotic macule |
|
| Oral congenital melanocytic nevi |
|
| Peutz-Jeghers syndrome |
|
| Laugier-Hunziker syndrome |
|
| Addison’s disease |
|
| Oral acanthosis nigricans |
|
| Oral hairy leukoplakia |
|
| Other differential diagnosis: amalgam tattoo, medication-induced hyperpigmentation, melanoacanthoma | |
Characteristic ‘hairy’ appearance of the dorsum of the tongue, sparing the rest of the oral cavity, including its lateral and anterior borders, makes BHT a straightforward diagnosis. Dermoscopy has been used to aid in the diagnosis as a non-invasive alternative to scraping.3
Management guidelines during infancy, where other contributing factors are ruled out, is the reassurance of worried parents regarding the benign and self-resolving nature of this condition. Better oral hygiene and gentle tongue scraping can promote desquamation.3 Though lacking sufficient evidence, topical retinoid, urea, trichloroacetic acid, salicylic acid and gentian violet have also been suggested in adult BHT.3,8
Discoloured tongue or chromoglossia in an infant will always be a cause of worry for new parents but careful examination will ease a clinician to arrive at the diagnosis.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
References
- A case of lingua villosa nigra (black hairy tongue) in a 3-month-old infant. Am J Case Rep. 2020;21:e926362.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Black hairy tongue syndrome. World J Gastroenterol. 2014;20:10845-50.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Black hairy tongue: predisposing factors, diagnosis, and treatment. Am J Clin Dermatol. 2017;18:563-9.
- [CrossRef] [PubMed] [Google Scholar]
- Black hairy tongue in a 2-month-old infant. J Paediatr Child Health. 2008;44:377-9.
- [CrossRef] [PubMed] [Google Scholar]
- Black and Brown: Non-neoplastic pigmentation of the oral mucosa. Head Neck Pathol. 2019;13:47-55.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Hyperpigmented macules of the tongue in a 15-year-old girl. Pediatr Dermatol. 2021;38:941-2.
- [CrossRef] [PubMed] [Google Scholar]
- oral congenital melanocytic nevus: A rare case report and review of the literature. Head Neck Pathol. 2015;9:481-7.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]





