Translate this page into:
Lymphangiectasia of the vulva, treatment with CO 2 laser
Correspondence Address:
Myriam Ben Hamida
Service de Dermatologie,H�pital Charles Nicolle, Bureau Entr�es Boulevard du 9 Avril 1006, BAB SOUIKA TUNIS, Tunisie
| How to cite this article: Hamida MB, Baccouche D, El Fekih N, Fazaa B, Kamoun R. Lymphangiectasia of the vulva, treatment with CO 2 laser. Indian J Dermatol Venereol Leprol 2012;78:122 |
Sir,
Lymphangiectasia is a pathological dilatation of lymphatic vessels. Vulvar presentation is uncommon and may be misdiagnosed as genital warts, molluscum contagiosum, or tuberculosis verrucosa cutis. We present here the first case reported of vulval lymphangiectasia associated with a benign pelvic tumor.
A 55-year-old woman, presented with vulvar itching associated with condyloma-like lesions, starting 2 years ago. There was a medical history of hypertension and dyslipidemia under treatment. There were no histories of sexually transmitted disease, filariasis, tuberculosis, trauma, Crohn′s disease, pelvic surgery, or irradiation therapy. The clinical examination revealed a diffuse induration with verrucous appearance of both labia major, with overlying papulovesicular lesions [Figure - 1]. There was no inguinal lymphadenopathy. Histological examination revealed, the presence in the papillary dermis, of multiple dilated lymphatic vessels, lined by a thin wall comprising of endothelial cells with valves. Acanthosis was also present in the epidermis [Figure - 2]. The diagnosis of vulval lymphangiectasia was proposed. An extensive search for an etiology of this disease in our patient was initiated. The searches for tuberculosis and for a sexually transmitted disease (especially Chlamydia serology) were negative. Abdominopelvic ultrasound revealed a large polymyomatous uterus, with multiple interstitial myomas measuring from 2 to 8 cm of diameter. A pelvic magnetic resonance imaging (MRI) was performed and confirmed the presence of large myomas, without deep pelvic extension of lymphangioma. Because there were no other obvious causes, we considered that this benign pelvic tumor was the cause of the impaired lymph flow inducing lymphangiectasia. Surgical treatment represented by total hysterectomy was performed. For her vulval lymphangiectasia, a noninvasive therapy with CO 2 -laser vaporization was indicated. The continuous wave CO 2 laser was used in defocused mode with a 2-mm spot size. The patient had two laser sessions at 4 weeks interval, with a power of 10 W. The evolution was favorable with a good cosmetic result and no signs of recurrence after 15-month follow-up [Figure - 3].
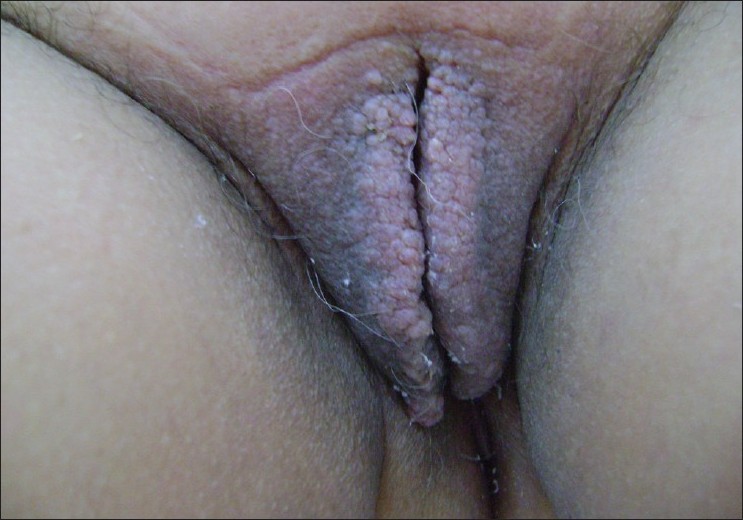 |
| Figure 1: Verrucous appearance of both labia major a with overlying papulo-vesicular lesions |
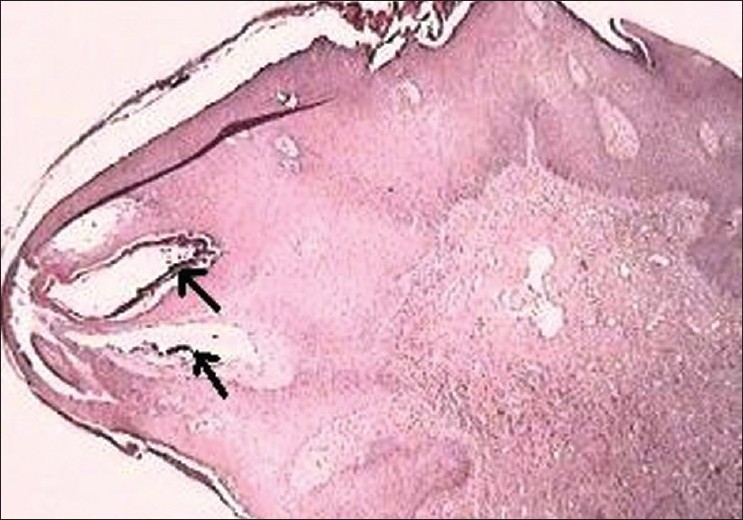 |
| Figure 2: Multiple dilated lymphatic vessels in the papillary dermis (H and E, ×100) |
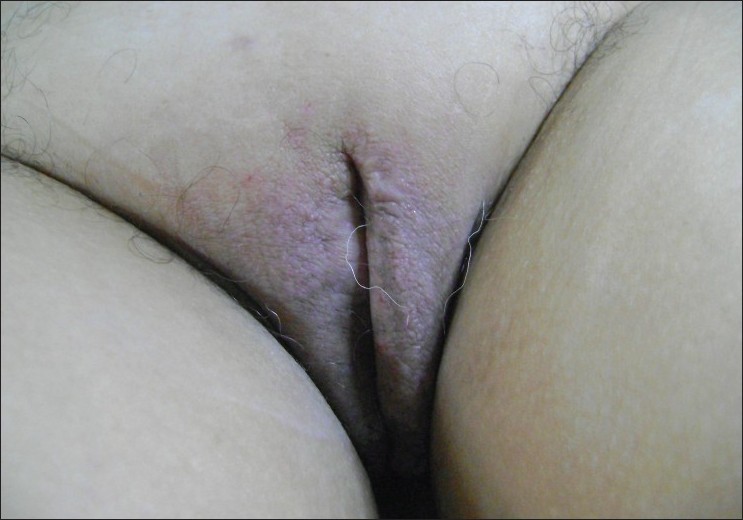 |
| Figure 3: Evolution after 15 months-follow-up |
We report here an original case of vulval lymphangiectasia caused by a large polymyomatous uterus. Lymphangiectasia is also called acquired lymphangioma circumscriptum (LC) or secondary lymphangiomas. Requena and Sangueza [1] consider that this disorder results from obstruction of previously normal lymphatics, unlike congenital LC in which dilated superficial lymphatics are a consequence of transmitted pressure from a congenital malformation of deep dermal lymphatics.
Clinical and histological findings of lymphangiectasia and congenital LC of the vulva are very similar. However, history of congenital or early onset of the disease and the presence on histological examination of deeper lymphatic abnormalities in the reticular dermis and subcutaneous are suggestive of LC. [2]
For our patient, the late onset of the disease and the absence of deep lymphatic extension on histological examination and on pelvic MRI were suggestive of lymphangiectasia of the vulva.
In the literature, vulval lymphangiectasia occurred after a carcinoma of the cervix uteri managed with surgery or with radiation therapy. Other predisposing conditions reported were urogenital tuberculosis, Crohn′s disease, recurrent bacterial infections, or radical pelvic surgery of non-gynecologic tumors. [3] In all these cases, lymphangiectasia was induced by obstruction of previous normal lymphatics. To the best of our knowledge, it is the first case of vulval lymphangiectasia associated with a benign pelvic tumor. We propose that these large myomas were probably the cause of the impaired lymph flow inducing lymphangiectasia.
There is no consensus about the treatment of lymphangiectasia. Treatment must provide a good cosmetic result, prevent recurrence, and protect from infections. The traditional treatment, surgical removal, is an effective treatment but rapid relapses often occur. Other treatment options include laser vaporization, sclerotherapy, cryotherapy, and electrocoagulation. Several reports have been published of successful CO 2 laser ablation of lymphangiectasia, and it represents the main alternative to surgery. [2] The CO 2 laser is described as effective in both LC and lymphangiectasia; however, focal recurrence are more frequently described in LC, which may reflect the persistence of deeper lymphatic abnormalities not destroyed by laser. [2] CO 2 laser ablation is generally well tolerated but some authors noted pain and the development of vulva keloid. In our patient, a conservative treatment with CO 2 -laser therapy was indicated. This treatment was well tolerated with a good cosmetic result and no recurrence after a follow-up of 15 months.
Malignant transformation of congenital LC has been reported in some cases from the literature. Cases of lymphangiosarcoma were described on sites of LC previously treated with extensive X-ray therapy. [4]
Cases of squamous-cell carcinoma have also been reported. [5] These complications have never been reported with lymphangiectasia; nevertheless, a close follow-up of patients with vulval lymphangiectasia is advisable.
| 1. |
Requena L, Sangueza OP. Cutaneous vascular anomalies. Part I. Hamartomas, malformations, and dilatation of preexisting vessels. J Am Acad Dermatol 1997;37:523-49.
[Google Scholar]
|
| 2. |
Huilgol SC, Neill S, Barlow RJ. Laser ablation of vulval lymphangiectasia and lymphangioma. Dermatol Surg 2002;28:575-7.
[Google Scholar]
|
| 3. |
Vlastos AT, Malpica A, Follen M. Lymphangioma circumscriptum of the vulva: A review of the literature. Obstet Gynecol 2003;101:946-54.
[Google Scholar]
|
| 4. |
King DT, Duffy DM, Hirose FM, Gurevitch AW. Lymphangiosarcoma arising from lymphangioma circumscriptum. Arch Dermatol 1979;115:969-72.
[Google Scholar]
|
| 5. |
Wilson GR, Cox NH, McLean N, Scott D. Squamous cell carcinoma arising within congenital lymphangioma circumscriptum. Br J Dermatol 1993;129:337-9.
[Google Scholar]
|
Fulltext Views
1,354
PDF downloads
2,655





