Translate this page into:
Relapsing linear acantholytic dermatosis in a four-year-old boy
2 Departments of Pathology, Base Hospital, Delhi Cantt-110010, India
Correspondence Address:
Sandeep Arora
Skin Centre, Base Hospital, Delhi Cantt-110 010
India
| How to cite this article: Arora S, Arora G, Ranjan P. Relapsing linear acantholytic dermatosis in a four-year-old boy. Indian J Dermatol Venereol Leprol 2005;71:351-353 |
Abstract
Linear acantholytic dermatoses are a spectrum of cutaneous disorders that form a subset of linear dermatoses with distinct clinical features and histopathologically show acantholysis. The lesions may be zosteriform or follow the lines of Blaschko. This report describes a four-year-old boy who, on a follow up of two years, exhibited a relapsing acantholytic dermatosis along the lines of Blaschko. Histopathology of a representative lesion revealed epidermal acantholysis with multiple acantholytic keratinocytes with in the prickle cell layer and an absence of corp ronds and grains, consistent with features of Hailey-Hailey disease. This, to our knowledge, is the third case of relapsing linear acantholytic dermatosis reported. |
 |
 |
 |
 |
 |
Introduction
Relapsing linear acantholytic dermatosis was first described as a distinct entity in 1985 as a form of linear dermatosis with recurrent vesiculation or erosions and histopathologically characterized by features suggestive of Hailey-Hailey disease.[1] Although a debate rages over the existence of such dermatosis as a separate entity or a forme fruste of localized Darier′s disease,[2],[3] we describe a four-year-old boy who exhibited recurrent papulo-erosive lesions distributed along the lines of Blaschko with histopathological evidence of acantholysis.
Case report
A four-year-old boy presented with recurrent erosions and occasional papulo-vesicles over the right side of the trunk, neck and upper limb since the age of six months. He typically developed exacerbations during the summer, with aggravation following secondary infection of the lesions. The rash used to subside with or without medication over the next 2-3 weeks, followed by a fresh crop. He was asymptomatic during the winter. There was no family history of similar lesions.
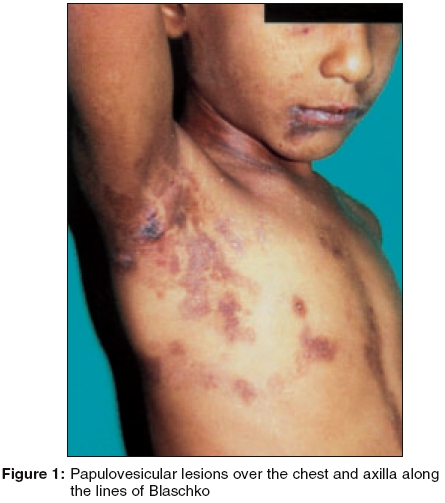
Examination revealed lesions distributed over the right side of the body. Multiple erosions and a few papulo-vesicular lesions, some with crusting and secondary impetiginization, were arranged in a linear fashion over the back, anterior chest wall and right axillary region. Multiple hyperpigmented streaks reminiscent of post-inflammatory hyperpigmentation were observed along the lines of Blaschko over the right arm and forearm, right side of trunk and right axillary regions with a sharp midline cut-off [Figure - 1]. The palms, soles and mucosae were normal.
Histopathology [Figure - 2] and [Figure - 3] one such lesion on the right shoulder showed epidermal acantholysis with multiple acantholytic keratinocytes within the prickle cell layer. Corp ronds and grains were not visible. The dermis contained a nonspecific inflammatory infiltrate.
The patient was followed up for two years. He was managed symptomatically with sun avoidance during summer, which helped in reducing the severity of eruptions and with topical antibiotics for secondary impetiginization.
Discussion
Relapsing linear acantholytic dermatosis is morphologically similar to Hailey-Hailey disease with exacerbation following sun exposure and local infections. The onset was initially reported in infancy,[1] but Duschet et al[4] reported an 81-year-old man with similar lesions. Our patient had an onset similar to the case reported by Vakilzadeh and Kolde,[1] but he had no family history of similar lesions.
The differential diagnosis in such a case of linear acantholytic dermatosis includes localized Darier′s disease,[5] Grover′s disease with a zosteriform distribution,[6] acantholytic dyskeratotic epidermal nevus[7],[8] and nevus corniculatus.[9] The absence of palmoplantar and nail involvement, no predilection for seborrheic areas, and absence of dyskeratotic cells, corp ronds and grains on histopathology in our patient were distinguishing features from a localized form of Darier′s disease. Acantholytic dyskeratotic epidermal nevus and nevus corniculatus have been typically described with hyperkeratotic papules and plaques in a linear distribution with evident dyskeratosis on histopathology. Grover′s disease presents with pruritic papules and papulovesicles in a truncal distribution in middle age.
The concept of genetic mosaicism had been proposed by Happle for skin disorders following the lines of Blaschko.[10] A post-zygotic mutation may result in a single region of abnormal cells forming separate regions due to cell migration, which is a programmed direction of embryonic movement. This concept would probably explain the distribution of lesions in our patient.
| 1. |
Vakilzadeh F, Kolde G. Relapsing linear acantholytic dermatosis. Br J Dermatol 1985;112:349-55.
[Google Scholar]
|
| 2. |
Fantini F, Kovacs E, Scarabello A. Unilateral transient acantholytic dermatosis (Grover's disease) along Blaschko lines. J Am Acad Dermatol 2002;47:319-20.
[Google Scholar]
|
| 3. |
Happle R. Linear Darier's disease or Grover's disease? J Am Acad Dermatol 2003;49:1200-1.
[Google Scholar]
|
| 4. |
Duschet P, Happle R, Schwarz T, Gschnait F. Relapsing linear acantholytic dermatosis. J Am Acad Dermatol 1995;33:920-2.
[Google Scholar]
|
| 5. |
Boente Mdel C, Frontini Mdel V, Primc NB, Asial RA. Linear Darier disease in two siblings. An example of loss of heterozygosity. Ann Dermatol Venereol. 2004;131:805-9.
[Google Scholar]
|
| 6. |
Liss WA, Norins AL. Zosteriform transient acantholytic dermatosis. J Am Acad Dermatol 1993;29:797-8.
[Google Scholar]
|
| 7. |
Gilaberte M, Puig L, Vidal D, Alomar A. Acantholytic dyskeratotic naevi following Blaschko's lines: a mosaic form of Darier's disease. J Eur Acad Dermatol Venereol. 2003;17:196-9.
[Google Scholar]
|
| 8. |
Mazereeuw-Hautier J, Thibaut I, Bonafe JL. Acantholytic dyskeratotic epidermal nevus: a rare histopathologic feature. J Cutan Pathol. 2002;29:52-4.
[Google Scholar]
|
| 9. |
Happle R, Steijlen PM, Kolde G. Naevus corniculatus: a new acantholytic disorder. Br J Dermatol 1990;122:107-12.
[Google Scholar]
|
| 10. |
Happle R. Mosaicism in human skin: understanding the pattern and mechanisms. Arch Dermatol 1993;129:1460-70.
[Google Scholar]
|
Fulltext Views
2,348
PDF downloads
936





