Translate this page into:
The risk of herpes zoster in patients with psoriasis: A retrospective records-based observational study
Correspondence Address:
Matteo Megna
Department of Dermatology, University of Naples Federico II, Via Pansini, 5 80131 Napoli
Italy
| How to cite this article: Megna M, Napolitano M, Ayala F, Balato N. The risk of herpes zoster in patients with psoriasis: A retrospective records-based observational study. Indian J Dermatol Venereol Leprol 2016;82:744 |
Sir,
Biologic drugs have dramatically changed the course of chronic inflammatory diseases such as psoriasis. The common biologic agents used in psoriasis include tumor necrosis factor alpha inhibitors such as adalimumab, infliximab, golimumab (monoclonal antibodies), etanercept (dimeric fusion protein) and interleukin-12/23 inhibitors like ustekinumab.[1] With the rising evidence of their efficacy, these agents are being increasingly used in the management of psoriasis and psoriatic arthritis which has led to the need for better surveillance of their safety profiles. Particularly, patients undergoing treatment with biologics need to be closely monitored for symptoms or signs of infection.[2] The increased risk of severe bacterial infections in these patients, especially reactivation of tuberculosis, has received much attention in the past but the effect on viral infections has not been extensively investigated.[2],[3]
Varicella zoster virus is a member of the herpes virus family which establishes latency in the neural tissue following primary infection. Herpes zoster, a papulo-vesicular eruption occurring in a dermatomal pattern which is often associated with neuralgic pain, results from reactivation of the latent varicella zoster virus from the dorsal spinal root ganglia. There may be associated rare, but severe neurological complications including optic neuritis, aseptic meningitis and meningo-encephalitis. Limited studies have been published till date regarding the incidence of herpes zoster during therapy with biologic drugs, the results of which are controversial.[4],[5],[6],[7] For these reasons, we performed a retrospective records-based observational study on 502 psoriatic patients, investigating the potential risk of viral infection and/or reactivation related to the use of biologic treatments, particularly focusing on the incidence of herpes zoster.
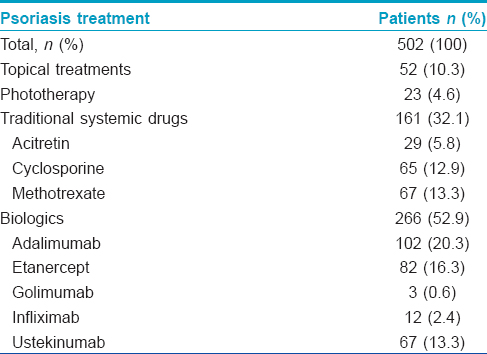
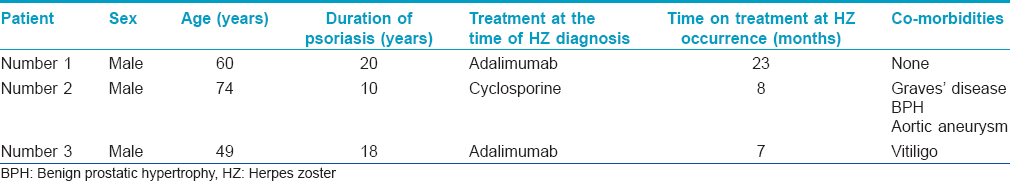
The study subjects were patients affected by psoriasis and/or psoriatic arthritis, attending the Psoriasis Care Center, Department of Dermatology, University of Naples Federico II, Italy, in the time period September 2010 to September 2013. The total study population comprised of 502 patients. The mean age of the subjects was 51.7 years (range 16–88 years), of whom 322 were males and 180, females. Almost 53% (n = 266) patients were on treatment with biologic drugs, whereas 32.1% (n = 161) subjects received traditional systemic therapies; detailed data regarding the treatment regimen followed in the study subjects is presented in [Table - 1]. Only three patients (0.6%), all males, developed herpes zoster during the psoriasis treatment period [Table - 2]. The mean age of the patients who developed herpes zoster was 61 years (range 49–74), comparable to the general population. No cases of atypical, bidermatomal and/or multidermatomal herpes zoster or persistent post-zoster neuralgia were observed. As regards the type of treatment administered to the patients who had an episode of herpes zoster during the course of psoriasis, two subjects developed herpes zoster during treatment with adalimumab and one patient with cyclosporine. Our data showed that the prevalence of herpes zoster in psoriasis patients was not higher than in the general population (1.5–3.5/1000 person-years).[8] Moreover, the risk of developing herpes zoster in psoriasis patients seemed not significantly influenced by treatment; in particular, we observed a similar proportion of cases in the biologic and traditional systemic drug groups (n = 2/266; 0.0075% vs. n = 1/166; 0.0063%, respectively). Studies regarding the incidence of herpes zoster in psoriasis patients are still scanty and the risk of herpes zoster associated with the use of biologics in these patients remains controversial. To conclude, our retrospective records-based observational study showed no significant increase in the risk of developing herpes zoster in psoriasis patients under treatment with biologics or traditional systemic drugs. Moreover, no cases of atypical, severe and/or multidermatomal forms of herpes zoster were seen associated with the use of these drugs.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Ghasri P, Yamauchi PS. The role of methotrexate in the era of biological therapies for treating psoriasis. Adv Psoriasis Inflamm Skin Dis 2010;2:39-45.
[Google Scholar]
|
| 2. |
Isaacs D. Infectious risks associated with biologics. Adv Exp Med Biol 2013;764:151-8.
[Google Scholar]
|
| 3. |
Domm S, Cinatl J, Mrowietz U. The impact of treatment with tumour necrosis factor-alpha antagonists on the course of chronic viral infections: A review of the literature. Br J Dermatol 2008;159:1217-28.
[Google Scholar]
|
| 4. |
Adelzadeh L, Jourabchi N, Wu JJ. The risk of herpes zoster during biological therapy for psoriasis and other inflammatory conditions. J Eur Acad Dermatol Venereol 2014;28:846-52.
[Google Scholar]
|
| 5. |
Failla V, Jacques J, Castronovo C, Nikkels AF. Herpes zoster in patients treated with biologicals. Dermatology 2012;224:251-6.
[Google Scholar]
|
| 6. |
Di Costanzo L, Ayala F, Megna M, Gaudiello F, Patrì A, Balato N. The risk of herpes zoster in the anti-TNF-a era: A case report and review of the literature. J Dermatol Case Rep 2013;7:1-4.
[Google Scholar]
|
| 7. |
Dreiher J, Kresch FS, Comaneshter D, Cohen AD. Risk of Herpes zoster in patients with psoriasis treated with biologic drugs. J Eur Acad Dermatol Venereol 2012;26:1127-32.
[Google Scholar]
|
| 8. |
Gnann JW Jr, Whitley RJ. Clinical practice. Herpes zoster. N Engl J Med 2002;347:340-6.
[Google Scholar]
|
Fulltext Views
1,141
PDF downloads
1,576





