Translate this page into:
Transient dermatoses: Leaving a lasting memory
Corresponding author: Dr. Anupam Das, Department of Dermatology, KPC Medical College and Hospital, Kolkata, West Bengal, India. anupamdasdr@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Das A, Sil A, Khullar G. Transient dermatoses: Leaving a lasting memory. Indian J Dermatol Venereol Leprol 2022;88:265-7.
Introduction
The Oxford English dictionary defines transient as “for a short time only or not lasting, enduring, or permanent.” However, such fleeting experiences are often enough to chalk out a lasting impression in the mind of an astute clinician. This holds especially true in the field of dermatology, where visual impressions form the backbone of clinical diagnosis. Being acquainted with such evanescent clues would make our job of reaching an appropriate diagnosis and treatment, a much smoother task. This article is meant to refamiliarize dermatologists with some newly coined dermatoses bearing the terminology “transient.”
Transient acantholytic dermatosis: Also known as Grover’s disease,1 it is characterized by the development of pruritic, papulovesicular eruptions over the trunk (anterior part of chest and upper part of back) and proximal extremities. Heat, sweating, atopic dermatitis and asteatotic dermatitis have been thought to be aggravating factors. Histological features include focal acantholysis, dyskeratosis and spongiosis.2 Therapeutic options include potent topical steroids, oral retinoids, chemical peeling, cryotherapy and phototherapy;3-5 however, recurrence is commonly observed.
Transient neonatal pustular melanosis: It is a benign, idiopathic dermatosis seen in newborns and presents with vesicles, superficial pustules and pigmented macules.6 Based on the time of the examination, the lesions may be found predominantly over the chin, neck, forehead, on the retroauricular region, palms and soles. The vesicopustules resolve within 1–2 days, and the hyperpigmented macules disappear within a month. Histology of vesiculopustules shows intraepidermal collection of neutrophils and eosinophils,7 whereas the pigmented macules show melanization of the basal layer. Treatment is usually not required.
Transient aquagenic wrinkling of palms: It is a transient condition affecting predominantly young females. Clinically, it presents with whitish papules, edema and increased wrinkling of palms which gets aggravated with immersion of hands in water; with spontaneous resolution within 20 min. Histology shows spongiosis and dilation of eccrine acrosyringia.8 It has been found to be associated with cystic fibrosis,9 focal hyperhidrosis and Raynaud’s phenomenon.
Transient lingual papillitis: First described in 1996,10 it is an acute onset, transient and painful hyperplasia of fungiform lingual papillae. The risk factors for the development of this condition are acute or chronic mechanical trauma, stress, lack of sleep, poor nutrition, geographic tongue, excessive smoking and alcohol intake.11 Treatment is essentially symptomatic and involves the administration of local anesthetics, topical corticosteroids, coating agents and saline mouthwashes.12
Transient neonatal hair loss: This is the other name given to neonatal occipital alopecia, and the authors had proposed the term transient neonatal hair loss,13 because the location of alopecia is not occipital in all the cases. This is commonly seen during the 2nd month of life in neonates. For many years, neonatal occipital alopecia has been attributed to friction caused by the sleeping position of the neonate. It clinically manifests with a well-defined, elongated to oval patch of alopecia, the main diameter extending from one auricular pavilion to the other [Figure 1]. It is now proposed that transient neonatal hair loss has no relationship with sleep position, rather it is the physiological shedding of hair (telogen hair falling off).14
Transitory contractile dermatoses: First described by Torrelo et al. as “infantile transient smooth muscle contraction of the skin,”15 authors reported a transient rippling of the skin of lower limbs triggered by minimal cold exposure or friction in otherwise healthy neonates. Most of the cases resolved spontaneously within two years of life. This was attributed to transient contraction of the arrector pili smooth muscle fibers in the skin, caused by immaturity of the autonomic nervous system, primitive reflex phenomenon or transient hypersensitivity of the smooth muscle. The predilection for lower limbs remains unexplained. The term “transient contractile dermatosis” was proposed by Rizvi and Helsing,16 when the authors came across a similar case. However, the report was subsequently questioned later. The authors asserted that the case reported by Rizvi and Helsing were induced by vigorous rubbing and pinching, and the original cases described in 2013 as “infantile transient smooth muscle contraction of the skin”16 were spontaneous in onset and disappeared with age.17
Transient pigmentary lines of the newborn: Originally described by Gibbs18 in 1967 in a male infant, it presents with linear streaks of hyperpigmentation on the back, abdomen, knees, legs, etc. The etiology is not clear, however, this could be due to mechanical trauma from hyperkeratosis within the folds, probably because of in utero flexion position, leading to post-inflammatory hyperpigmentation. This is a self-limiting condition and does not require treatment.19
Transient neonatal zinc deficiency: It develops in breastfed infants due to low zinc concentration in the milk of the nursing mothers. Clinically, it manifests with dermatitis, alopecia, decreased growth and impaired immune function. It is inherited in an autosomal dominant pattern.20 Treatment usually relies on zinc supplementation, however infants do not require zinc supplementation following weaning and have normal zinc absorption, unlike acrodermatitis enteropathica (severe form of zinc deficiency) where zinc supplements are needed lifelong.21
Transient bullous dermolysis of newborn: First described in 1985,22 it is a rare variant of dystrophic epidermolysis bullosa characterized by generalized blistering at birth, due to a mutation in type VII collagen gene (COL7A1). Clinical features include blisters all over the body followed by development of milia, atrophy, scarring and nail dystrophy. Histology typically reveals subepidermal blistering. It usually regresses within the first two years. Genetic counseling plays a pivotal role in the management of this condition.23
Transient porphyrinemia: It is an uncommon dermatological condition presenting with a photodistributed erythematous, violaceous or purpuric appearing eruption, developing within 1–5 days of phototherapy (6–10). The condition improves once phototherapy is discontinued.24 It is hypothesized that transiently elevated porphyrin levels in the skin absorb visible light during exposure to phototherapy, leading to the development of a photo-induced cutaneous eruption.25
Vesiculopustular eruption in transient myeloproliferative disorder of Down syndrome: A characteristic vesiculopustular eruption occurs in neonates with trisomy 21 or mosaicism for trisomy 21. This is seen in the setting of transient myeloproliferative disorder, a congenital leukemoid reaction that affects approximately 10% of babies with Down syndrome.26 Vesicles and pustules are predominately situated over the face, but may involve the trunk, extremities and sites of minor trauma as a consequence of pathergy, characterized by the development of discrete papules secondary to trauma.26 Histopathology demonstrates intraepidermal spongiotic vesiculopustules, the infiltrate being composed of immature myelocytes and promyelocytes with some mature neutrophils. The skin lesions tend to resolve spontaneously within weeks to months following subsidence of the leukemoid reaction. However, affected patients should be under regular pediatric oncology consultation due to an increased risk of the development of myeloid leukemia.27
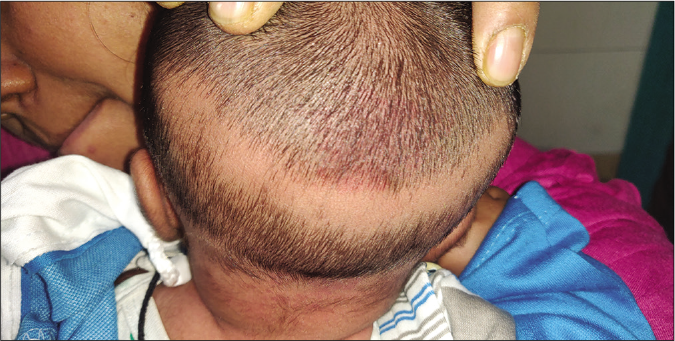
- Elongated oval patch of alopecia on the occiput of a neonate
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Transient acantholytic dermatosis. Arch Dermatol. 1970;101:426-34.
- [CrossRef] [PubMed] [Google Scholar]
- Distinguishing histopathologic features of acantholytic dermatoses and the pattern of acantholytic hypergranulosis. J Cutan Pathol. 2019;46:6-15.
- [CrossRef] [PubMed] [Google Scholar]
- Grover's disease treated with isotretinoin. Report of four cases. J Am Acad Dermatol. 1985;12:981-4.
- [CrossRef] [Google Scholar]
- Effective treatment of persistent Grover's disease with trichloroacetic acid peeling. Dermatol Surg. 2006;32:1083-8.
- [CrossRef] [PubMed] [Google Scholar]
- Treatment of transient acantholytic dermatosis with liquid nitrogen. JAAD Case Rep. 2020;6:341-3.
- [CrossRef] [PubMed] [Google Scholar]
- Diagnosis and treatment of pustular disorders in the neonate. Pediatr Dermatol. 1997;14:131-43.
- [CrossRef] [PubMed] [Google Scholar]
- Transient reactive papulo translucent acrokeratoderma. J Am Acad Dermatol. 1996;34:686-7.
- [CrossRef] [Google Scholar]
- Aquagenic wrinkling of the palms in patients with cystic fibrosis homozygous for the delta F508 CFTR mutation. Arch Dermatol. 2005;141:621-4.
- [CrossRef] [PubMed] [Google Scholar]
- Transient lingual papillitis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1996;82:441-5.
- [CrossRef] [Google Scholar]
- Transient lingual papillitis: A retrospective study of 11 cases and review of the literature. J Clin Exp Dent. 2017;9:e157-62.
- [CrossRef] [PubMed] [Google Scholar]
- Transient neonatal hair loss: A common transient neonatal dermatosis. Eur J Pediatr. 2005;164:630-2.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence and factors associated with neonatal occipital alopecia: A retrospective study. Ann Dermatol. 2011;23:288-92.
- [CrossRef] [PubMed] [Google Scholar]
- Infantile transient smooth muscle contraction of the skin. J Am Acad Dermatol. 2013;69:498-500.
- [CrossRef] [PubMed] [Google Scholar]
- Transitory contractile dermatosis--a new entity? J Am Acad Dermatol. 2014;71:197.
- [CrossRef] [PubMed] [Google Scholar]
- Reply to transitory contractile dermatosis--a new entity? J Am Acad Dermatol. 2014;71:197-8.
- [CrossRef] [PubMed] [Google Scholar]
- Unusual striped hyperpigmentation of the torso. A sequel of abnormalities of epitrichial exfoliation. Arch Dermatol. 1967;95:385-6.
- [CrossRef] [PubMed] [Google Scholar]
- Transient pigmentary lines of the newborn. Pediatr Dermatol. 2009;26:768.
- [CrossRef] [PubMed] [Google Scholar]
- Identification of a mutation in SLC30A2 (ZnT-2) in women with low milk zinc concentration that results in transient neonatal zinc deficiency. J Biol Chem. 2006;281:39699-707.
- [CrossRef] [PubMed] [Google Scholar]
- Transient neonatal zinc deficiency in exclusively breastfed preterm infants. J Paediatr Child Health. 2018;54:319-22.
- [CrossRef] [PubMed] [Google Scholar]
- Transient bullous dermolysis of the newborn. Arch Dermatol. 1985;121:1429-38.
- [CrossRef] [PubMed] [Google Scholar]
- Transient bullous dermolysis of the newborn in three generations. Br J Dermatol. 2005;153:1058-63.
- [CrossRef] [PubMed] [Google Scholar]
- Transient porphyrinemia in a neonate: A case report. Pediatr Dermatol. 2016;33:e375-6.
- [CrossRef] [PubMed] [Google Scholar]
- Phototherapy induced cutaneous eruption in a neonate with transient porphyrinemia. J Neonatal Perinatal Med. 2015;8:417-20.
- [CrossRef] [PubMed] [Google Scholar]
- Vesiculopustular eruptions in Down syndrome neonates with myeloproliferative disorders. Arch Dermatol. 2001;137:760-3.
- [Google Scholar]
- Neonatal vesiculopustular eruption in Down syndrome and transient myeloproliferative disorder: A case report and review of the literature. Pediatr Dermatol. 2019;36:702-6.
- [CrossRef] [PubMed] [Google Scholar]





