Translate this page into:
Trichilemmal carcinoma in a young adult
2 Dermatology and Cutaneous Biology Research Institute, Yonsei University College of Medicine, Seoul, Republic of Korea
Correspondence Address:
Mi Ryung Roh
Department of Dermatology, Yonsei University College of Medicine 211 Eonjuro, Gangnam-gu, Seoul 135-720
Republic of Korea
| How to cite this article: Lee NR, Oh SJ, Roh MR. Trichilemmal carcinoma in a young adult. Indian J Dermatol Venereol Leprol 2015;81:531-533 |
Sir,
Trichilemmal carcinoma is an uncommon malignant cutaneous adnexal tumor derived from the external root sheath of hair follicle. The tumor usually manifests in the elderly as a solitary exophytic, polypoid, ulcerated nodule of less than 3 cm size, with a 3:1.6 female-male ratio. [1] It is usually found on sun-exposed areas. Here we report a solitary trichilemmal carcinoma discovered in a young healthy adult and review the etiology, histopathologic characteristics, differential diagnosis and treatment.
A 21-year-old man presented with a 3-month history of a slowly developing mass on his scalp. The lesion appeared as a 2.0 × 2.0 cm sized, slightly erythematous, hard, subcutaneous nodule with mild tenderness [Figure - 1]. There was neither a history of chronic sun exposure, nor a personal/family history of other cutaneous neoplasms. No abnormality was found in complete blood count, blood chemistry, urinalysis and syphilis reagin test. The tumor was removed by simple excision.
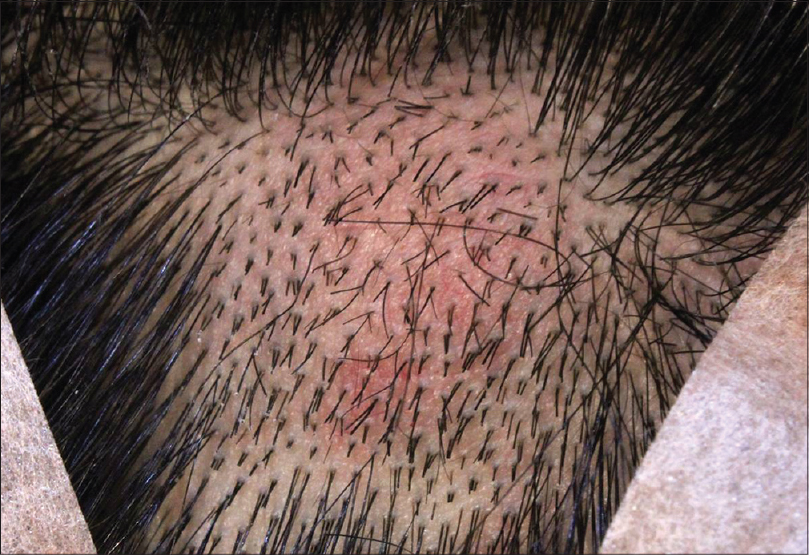 |
| Figure 1: A 2.0 × 2.0 cm sized, slightly erythematosus, mildly tender subcutaneous hard nodule on the scalp |
Histopathological examination revealed a well circumscribed epithelial tumor infiltrating the entire dermis in a lobular and trabecular pattern [Figure - 2]a. Foci of trichilemmal keratinization characterized by compact abrupt keratinization with absent granular layer were also present [Figure - 2]b and c. The tumor was composed of polygonal cells with eccentric nuclei and abundant clear cytoplasm with a peripheral palisade of basaloid cells [Figure - 2]d. Some tumor cells exhibited bizarre and pleomorphic nuclei with many mitotic figures [Figure - 3]. No special staining or immunohistochemical staining was done. The resection margins were clear of tumour cells and the patient was warned about malignant features of the tumor. However, the patient was subsequently lost to follow-up.
 |
| Figure 2: (a) A well circumscribed epithelial tumor infiltrating the entire dermis in a lobular and trabecular pattern (H and E, ×20). (b, c) Foci of trichilemmal keratinization characterized by compact abrupt keratinization with absent granular layer were also present (H and E, ×100). (d) The tumor was composed of polygonal cells with eccentric nuclei and abundant clear cytoplasm, with a peripheral palisade of basaloid cells (H and E, ×400) |
 |
| Figure 3: (a, b) Some tumor cells exhibited bizarre and pleomorphic nuclei with many mitotic figures (arrowhead) (H and E, ×100, H and E, ×200) |
Histologically, trichilemmal carcinoma manifests characteristic features. The tumor usually infiltrates the entire dermis in a trabecular and lobular pattern. Trichilemmal type keratinization characterized by absence of granular layer is seen focally. Tumor cells have large, clear glycogen-rich cytoplasm which is periodic acid-schiff (PAS)-positive, diastase-sensitive and mucin negative. Immunohistochemically, the tumor cells are reported to strongly express keratins (AE1/AE3), p63 nuclear protein, low molecular weight cytokeratin (cytokeratin 1, 5, 10, 14), and epithelial membrane antigen, [2] but are negative for carcinoembryonic antigen, S-100 protein and cytokeratin 17. [3]
Trichilemmal carcinoma must be differentiated from other skin cancers such as clear cell basal cell carcinoma, squamous cell carcinoma, malignant clear cell hidradenoma, sebaceous carcinoma and malignant proliferating trichilemmal tumor. Clear cell basal cell carcinoma lacks areas infiltrated by clear cells and is usually accompanied by areas of conventional basal cell carcinoma. Squamous cell carcinoma differs from trichilemmal carcinoma in the absence of trichilemmal keratinization or lobular proliferation, and in being periodic acid-schiff-negative. [4] Malignant clear cell hidradenoma can be distinguished from trichilemmal carcinoma by the absence of peripheral palisading and the presence of acinar or ductal differentiation, which can be demonstrated by positive carcinoembryonic antigen. [1] Sebaceous carcinoma is distinguished by the presence of sebaceous differentiation within tumour cells, which have a foamy, lipid-rich cytoplasm with a centrally located nucleus. [1] Malignant proliferating trichilemmal tumor is differentiated from trichilemmal carcinoma by the fact that it shows a lobular proliferation centered on the pilosebaceous unit with basilar or full thickness interfollicular epidermal spread, always connected to the epidermis. This tumor is also more prone to local recurrence and metastasis.
The pathogenesis of trichilemmal carcinoma remains unknown. Its distribution in sun-exposed areas suggests that actinic damage may contribute to its development. Misago et al. stated that trichilemmal carcinoma may develop de novo from actinically damaged skin, similar to squamous cell carcinoma. It has also been reported in a patient with xeroderma pigmentosa, [1] in patients with burn scars [5] and in a patient with long-term exposure to multiple chest radiographs for the management of pulmonary tuberculosis. [6] Immunosuppression and human papilloma viral infection are other possible contributing factors reported. [2] Additionally, malignant transformation from trichilemmoma has been postulated by Reis. [1] We found only 2 previous reports of trichilemmal carcinoma occurring in a young adult.
Trichilemmal carcinoma is reported to have an indolent clinical course. Simple excision with adequate margins is the treatment of choice for solitary trichilemmal carcinoma. Trichilemmal carcinoma was recently reported to have been treated with Mohs micrographic surgery [3],[4] . Multiple recurrences and metastasis to regional lymph nodes even after excision with clear resection margins has also been reported. [7] Although trichilemmal carcinoma has a low metastatic potential and rarely recurs, careful follow-up for early detection of recurrence is needed. A recent study suggested topical 5% imiquimod cream may be a promising therapeutic option for a patient for whom surgery is contradicted. [8]
| 1. |
Reis JP, Tellechea O, Cunha MF, Baptista AP. Trichilemmal carcinoma: Review of 8 cases. J Cutan Pathol 1993;20:44-9.
[Google Scholar]
|
| 2. |
Kanitakis J, Euvrard S, Sebbag L, Claudy A. Trichilemmal carcinoma of the skin mimicking a keloid in a heart transplant recipient. J Heart Lung Transplant 2007;26:649-51.
[Google Scholar]
|
| 3. |
Kim Y, Lee Y, Choi Y, Lee C, Kim K. A case of trichilemmal carcinoma treated with Mohs micrographic surgery. Ann Dermatol 2008;20:157-61.
[Google Scholar]
|
| 4. |
Lai TF, Huilgol SC, James CL, Selva D. Trichilemmal carcinoma of the upper eyelid.Acta Ophthalmol Scand 2003;81:536-8.
[Google Scholar]
|
| 5. |
Ko T, Tada H, Hatoko M, Muramatsu T, Shirai T. Trichilemmal carcinoma developing in a burn scar: A report of two cases. J Dermatol 1996;23:463-8.
[Google Scholar]
|
| 6. |
Chan KO, Lim IJ, Baladas HG, Tan WT. Multiple tumour presentation of trichilemmal carcinoma. Br J Plast Surg 1999;52:665-7.
[Google Scholar]
|
| 7. |
Kulahci Y, Oksuz S, Kucukodaci Z, Uygur F, Ulkur E. Multiple recurrence of trichilemmal carcinoma of the scalp in a young adult. Dermatol Surg 2010;36:551-4.
[Google Scholar]
|
| 8. |
Jo JH, Ko HC, Jang HS, Kim MB, Oh CK, Kwon KS. Infiltrative trichilemmal carcinoma treated with 5% imiquimod cream. Dermatol Surg 2005;31:973-6.
[Google Scholar]
|
Fulltext Views
2,904
PDF downloads
1,354





