Translate this page into:
Using a simple Jeweler's loupe as a dermoscopic instrument
Correspondence Address:
Feroze Kaliyadan
Department of Dermatology, Amrita Institute of Medical Sciences, Kochi, India
| How to cite this article: Kaliyadan F. Using a simple Jeweler's loupe as a dermoscopic instrument. Indian J Dermatol Venereol Leprol 2011;77:617-620 |
Sir,
Dermoscopy, also known as dermatoscopy, epiluminescence microscopy, surface microscopy, and incident light microscopy, is an in vivo noninvasive technique mainly used for the evaluation of pigmented lesions of the skin and accessible mucosa. When performed by an expert, it can significantly improve sensitivity and specificity of diagnosis of skin lesions, especially pigmented skin lesions. In the case of pigmented skin lesions, it helps in triage - both by early treatment of necessary cases and by avoiding unnecessary biopsies and excisions in benign conditions. [1] Dermoscopy is being increasingly used for easier and better diagnosis of a number of nonmelanocytic lesions, including benign lesions such as hemangiomas, basal cell carcinoma, seborrheic keratosis, actinic keratosis, Bowen′s disease, squamous cell carcinoma, etc. and even infections and infestations such as scabies and warts. [2],[3],[4]
The basic technique of dermoscopy involves the use of a device similar to an otoscope, which generates a beam of light that falls on the cutaneous surface ideally at an angle of 20°. Placing a fluid (oil, water, gel, alcohol-gel, or glycerin) at the interface between the epidermis and the device′s glass slide, eliminates reflection of light from the stratum corneum, allowing the visualization of the dermoscopic characteristics resulting from the presence of melanin and hemoglobin in the different skin layers. Newer polarized light dermoscopes do not require the use of fluid interfaces. The usual magnification provided by the dermoscope is 10-fold. [2]
One of the limitations of the widespread use of dermoscopy in countries such as India is the high cost of the equipment. The cost increases further if you add the price of a digital imaging system and required adapters for the same. We demonstrate how a simple jeweler′s loupe with an inbuilt light emitting diode (LED) light can be used as a dermoscope.
We used a simple Jeweler′s loupe with 10× magnification and an inbuilt LED light. Alcohol gel was used as the dermoscopy fluid. It should be noted that the lesions were viewed through the fluid with a small gap between the loupe and the fluid. In other words direct contact was not there. For recording the images a compact digital camera was used in macro mode with the camera lens manually held onto the viewing end of the loupe. Two common lesions are shown. The first lesion was a reticular nevus showing the typical dark brown regular pigment network [Figure - 1]a-d. [5] The second lesion was a cherry angioma showing the typical red "lacunae" associated with vascular lesions like hemangiomas [Figure - 2]a-d. [2] All images were recorded using a Sony DSC W-350 digital camera, in macro mode. The standard dermoscopy instrument used was a Dermlite® PRO HRII which has both polarized and fluid dermoscopy options. The cost for the Dermlite® PRO HRII device was around 900 US Dollars and the cost for the camera (with an adapter for Dermlite® PRO HRII) was 300 US Dollars. The cost of the jeweler′s loupe was less than 10 USD. The camera used for the imaging was the same in both instruments.
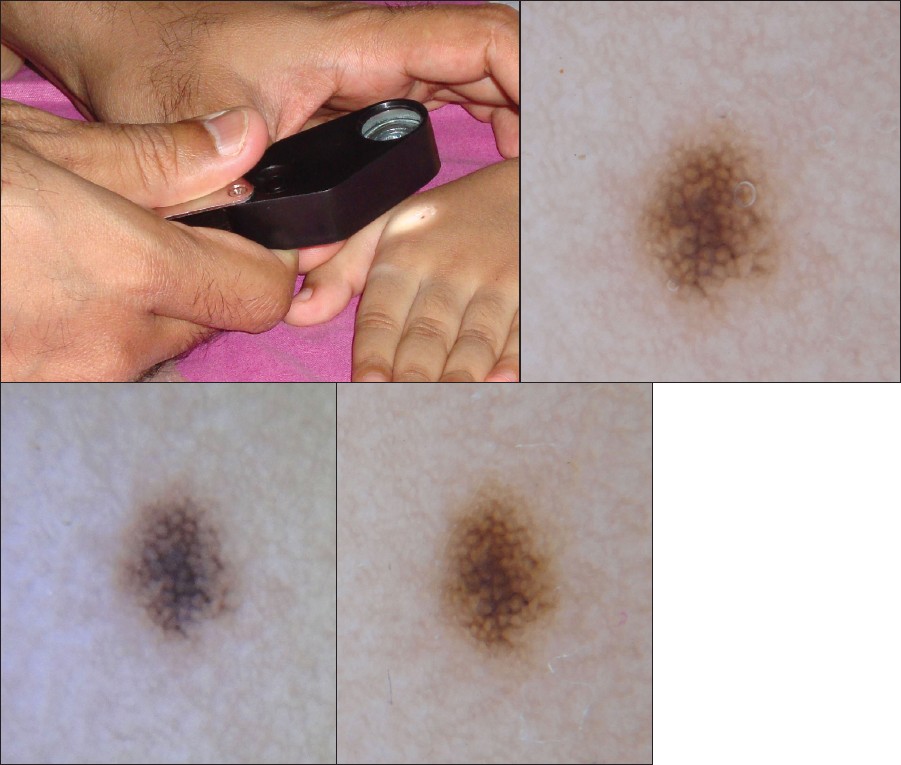 |
| Figure 1a: Examining a reticular nevus with a Jeweler's loupe with inbuilt LED light. Alcohol gel is used as the dermoscopy fluid Figure 1b: Reticular nevus - showing regular pigment network - fluid dermoscopy Dermlite® PRO HRII 10× Figure 1c: Reticular nevus - showing regular pigment network - fluid dermoscopy - Jeweler's loupe Figure 1d: Reticular nevus - showing regular pigment network - polarized light dermoscopy Dermlite® PRO HRII 10× |
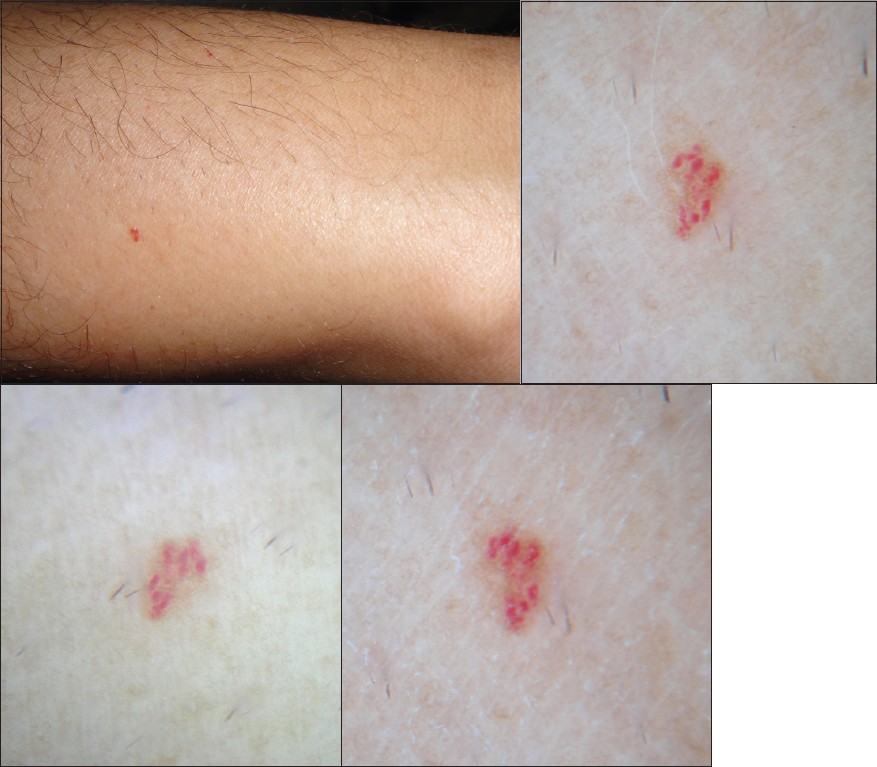 |
| Figure 2a: Cherry angioma forearm macro image Figure 2b: Cherry angioma fluid dermoscopy Dermlite® PRO HRII 10× Figure 2c: Cherry angioma fluid dermoscopy using Jeweler's loupe 10× Figure 2d: Cherry angioma polarized light dermoscopy Dermlite® PRO HRII 10× |
While the images no doubt indicate that the clarity is not as good as a proper dermoscope, most of the essential features of the studied skin lesions are easily discernible by this method also. One of the disadvantages, other than being a nonstandardized instrument, is that recording the images requires manually holding the camera on the loupe, while most modern dermoscopes have adapter systems to attach digital cameras, thus making it easier to record images. This combined with the lower precision of the lens could be a major hindrance is analyzing finer patterns like vascular patterns in some skin tumors. It should also be understood that the most important use of dermoscopy as of now continues to be in the diagnosis and triage of potentially malignant melanocytic lesions. Keeping this in mind, it would be premature to suggest an alternative method for this indication without extensive testing and validating of its results compared to conventional dermoscopy.
We would like to highlight that even a simple, cheap, and easily available instrument such as a jeweler′s loupe can be used as a low-cost dermoscopy device. This could especially be valuable in teaching basic dermoscopy concepts to dermatology residents.
| 1. |
Carli P, De Giorgi V, Soyer HP, Stante M, Mannone F, Giannotti B. Dermatoscopy in the diagnosis of pigmented skin lesions: A new semiology for the dermatologist. J Eur Acad Dermatol Venereol 2000;14:353-69.
[Google Scholar]
|
| 2. |
Campos-do-Carmo G, Ramos-e-Silva M. Dermoscopy: Basic concepts. Int J Dermatol 2008;47:712-19.
[Google Scholar]
|
| 3. |
Zalaudek I, Giacomel J, Cabo H, Di Stefani A, Ferrara G, Hofmann-Wellenhof R, et al. Entodermoscopy: A new tool for diagnosing skin infections and infestations. Dermatology 2008;216:14-23.
[Google Scholar]
|
| 4. |
Vazquez-Lopez F, Kreusch J, Marghoob AA. Dermoscopic semiology: Further insights into vascular features by screening a large spectrum of nontumoral skin lesions. Br J Dermatol 2004;150:226-31.
[Google Scholar]
|
| 5. |
Zalaudek I, Docimo G, Argenziano G. Using dermoscopic criteria and patient-related factors for the management of pigmented melanocytic nevi. Arch Dermatol 2009;145:816-26.
[Google Scholar]
|
Fulltext Views
2,943
PDF downloads
1,180





