Translate this page into:
Widespread cutaneous vasculopathy associated with levamisole-adulterated cocaine
Corresponding author: Prof. Alba Sanchez-Velazquez, Department of Dermatology, Hospital Universitario 12 de Octubre Avenida de Cordoba S/N, 28041, Madrid, Spain. als.velazquez@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Sánchez-Velázquez A, Calleja-Algarra A, Velasco-Tamariz V, Zarco-Olivo C. Widespread cutaneous vasculopathy associated with levamisole-adulterated cocaine. Indian J Dermatol Venereol Leprol 2021;87:540-2.
Sir,
A 53-year-old woman presented to the emergency department with a two day history of extensive, painful cutaneous lesions. Physical examination revealed patches of retiform purpura symmetrically affecting the upper arms, lower extremities, buttocks and abdomen, covering 40–45% of total skin surface area [Figure 1]. The patient was afebrile and hemodynamically stable. She reported regular cannabis use and occasional inhaled cocaine. Laboratory investigations revealed neutropenia (1600 cells/mm3), thrombocytopenia (110,000/mm3) and elevated C-reactive protein levels (13 mg/dL). Coagulation panel, liver function tests and urinalysis were unremarkable. Screening for lupus anticoagulant, anticardiolipin antibody and cryoglobulins was negative. Serological study was positive for antineutrophil cytoplasmic antibodies (c-ANCA) against proteinase three (PR3). Hepatitis viruses, syphilis and HIV tests were negative. Further workup ruled out infections and other etiologies of vasculitis. Urine drug test was positive for cocaine and cannabis. Histopathological examination revealed intraluminal thrombi within the superficial and deep dermal vessels. No inflammatory infiltrate was observed around the vessels. These findings were consistent with a thrombotic vasculopathy [Figure 2]. Therefore, based on the characteristic retiform cutaneous lesions, histological results and antineutrophil cytoplasmic antibodies positivity, a levamisole-induced vasculitis in a patient with a history of cocaine abuse was suspected. Despite treatment with systemic corticosteroids (1 mg/kg/day), skin lesions rapidly progressed to large confluent areas of necrosis and ulceration [Figure 3]. The patient was admitted to the burn intensive care unit to be closely monitored, ensure fluid replacement and supportive care and achieve better pain control with morphine. Colchicine and prophylactic systemic antimicrobial therapy were also initiated. The extension of the ulceration mandated surgical debridement of the necrotic tissue and coverage with skin grafts. Despite the severity of the cutaneous lesions, the patient remained hemodynamically stable and there was no evidence of systemic disease. Subsequently, she improved and was discharged in a good general condition.
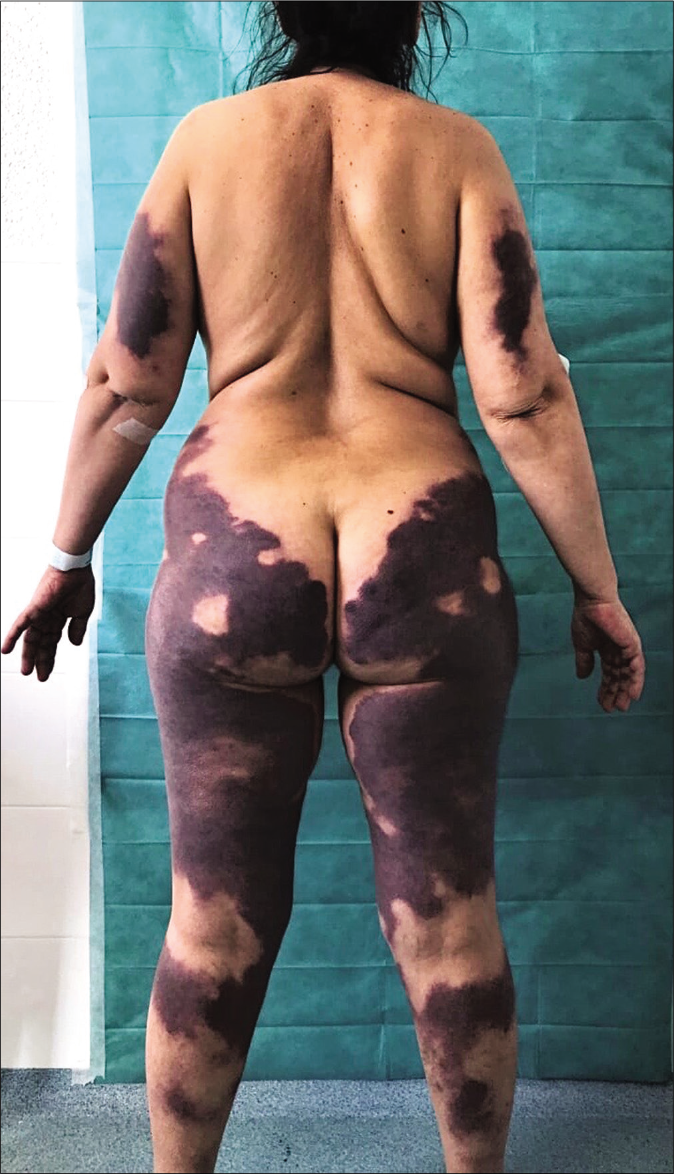
- Widespread violaceous patches of retiform purpura symmetrically affecting the upper and lower extremities and buttocks covering at least 40% of total body surface area
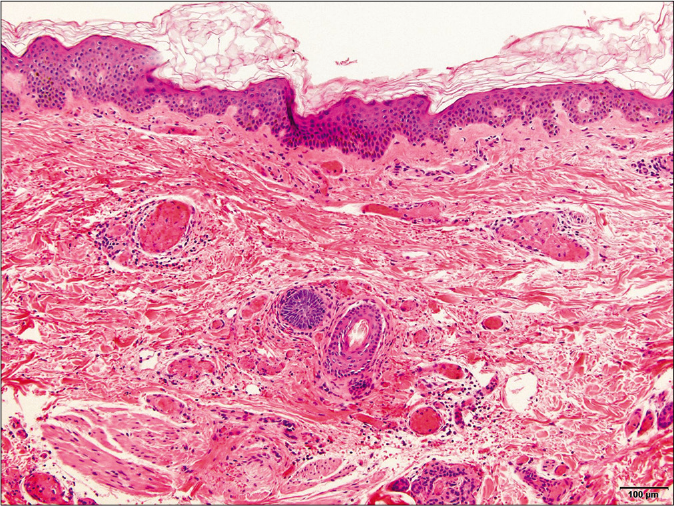
- Intraluminal thrombi within the superficial and deep dermal vessels. No inflammatory infiltrate was observed around the vessels. These findings were consistent with a thrombotic vasculopathy (H and E, ×100)
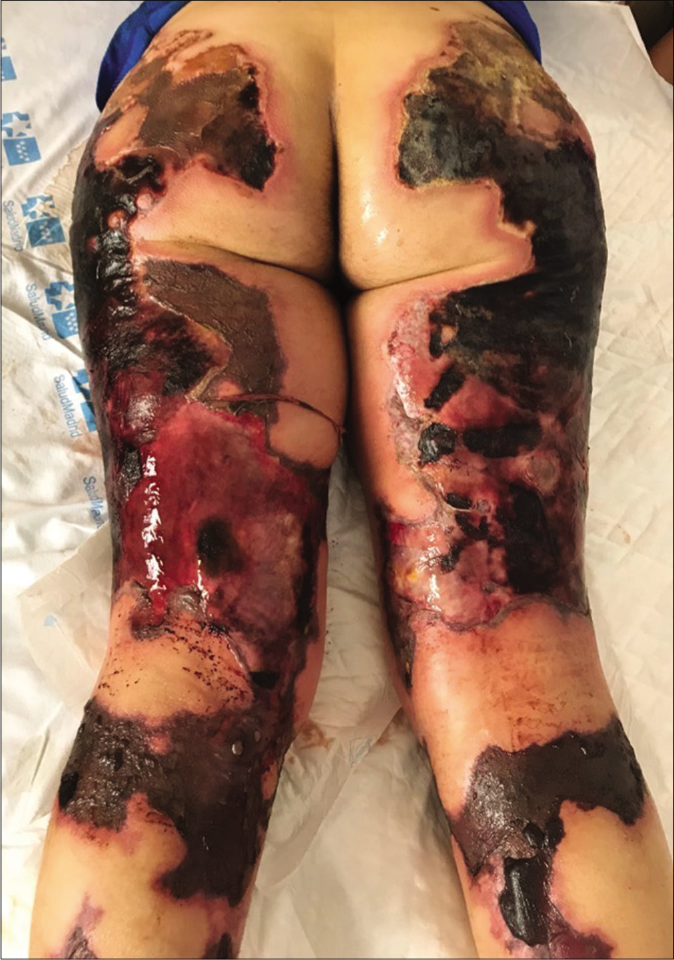
- Skin lesions rapidly progressed to large areas of necrosis and ulceration
Differential diagnosis of retiform purpura is broad and includes vasculitis, infectious and embolic phenomenon, warfarin induced skin necrosis, disseminated intravascular coagulation, cryoglobulinemia and anti-phospholipid antibody syndrome.1
A cutaneous vasculopathy syndrome has been described in users of cocaine contaminated with levamisole. This distinctive clinical entity is characterized by the presence of retiform purpura with a predilection for the ears and extremities, thrombosis of the small vessels, antineutrophil cytoplasmic antibodies positivity and leukopenia.2 Histologically, skin lesions demonstrate a thrombotic vasculopathy and/or leukocytoclastic vasculitis involving small- or medium-sized vessels. Accordingly, we established our diagnosis based on these criteria. Levamisole is the most common cocaine adulterant in Spain and all over the world. It was formerly used as an immunomodulatory agent for the treatment of autoimmune diseases and various cancers. The vast majority of cases of levamisole induced vasculitis in cocaine users did not have levamisole exposure confirmation. This link was based on the presence of levamisole in approximately 69% of the cocaine entering in the US2 and the typical clinical scenario. Moreover, its detection is difficult because not every center has the provision to test for levamisole using gas chromatography and mass spectrometry; besides, it has a short elimination half-life of 5.6 h. Consequently, many authors do not consider a positive test for levamisole necessary to establish the diagnosis of this syndrome.2 Finally, there are important clinical features that support the diagnosis of levamisole-contaminated cocaine-induced vasculopathy versus cocaine-induced vasculopathy. Vasculopathy due to levamisole has a very distinct presentation with purpuric lesions over the extremities and acral sites, neutropenia and p-ANCA or c-ANCA positivity. However, cocaine alone-induced vasculopathy does not present with ear necrosis, leukopenia or neutropenia and its typical mucocutaneous manifestations are cocaine-induced midline destructive lesions.
Due to the severity of the cutaneous lesions, our patient required intensive care nevertheless, she remained hemodynamically stable, there was no evidence of systemic disease, and she was discharged in a good general condition. On the contrary, most cases present with cutaneous lesions limited to the nose, ears, cheeks or thighs and experience resolution with the discontinuation of cocaine. Only a few cases of extensive necrosis have been described, however, most of them developed infectious complications and septicemia3-5 required amputations3,4 or eventually died.5 Surprisingly, in the current case, no systemic complications arose, and no amputations were needed. This is an unusual clinical evolution and it arises the idea that prognosis may be good, despite the extension of the cutaneous lesions. Dermatologists should keep in mind this clinical picture and the typical laboratory findings when assessing a retiform purpura and always rule out systemic complications such as renal failure, pulmonary hypertension, intra-alveolar hemorrhage or interstitial pneumonia5 which can lead to a fatal outcome.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- An approach to the patient with retiform purpura. Dermatol Ther. 2011;24:151-72.
- [CrossRef] [PubMed] [Google Scholar]
- A novel cutaneous vasculitis syndrome induced by levamisole-contaminated cocaine. Clin Rheumatol. 2011;30:1385-92.
- [CrossRef] [PubMed] [Google Scholar]
- A severe case of levamisole-induced vasculitis requiring extensive surgery and skin grafts. J Cutan Aesthet Surg. 2016;9:41-3.
- [CrossRef] [PubMed] [Google Scholar]
- Levamisole-adulterated cocaine leading to fatal vasculitis: A case report. Crit Care Nurse. 2017;37:49-57.
- [CrossRef] [PubMed] [Google Scholar]
- Systemic complications of levamisole toxicity. J Am Acad Dermatol. 2012;67:791-2.
- [CrossRef] [PubMed] [Google Scholar]





