Translate this page into:
Multiple xanthogranulomas in an adult
2 Department of Pathology, MKCG Medical College and Hospital, Berhampur, Orissa, India
Correspondence Address:
Surajit Nayak
Department of Skin and VD, MKCG Medical College, Berhampur - 760 010, Orissa
India
| How to cite this article: Nayak S, Acharjya B, Devi B, Patra MK. Multiple xanthogranulomas in an adult. Indian J Dermatol Venereol Leprol 2008;74:67-68 |
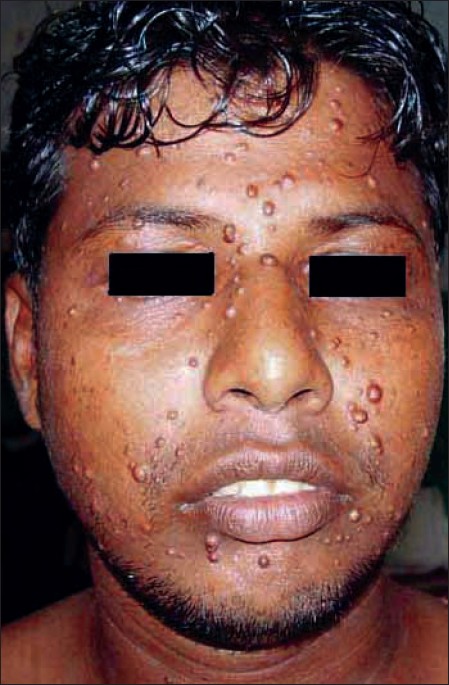 |
| Figure 1: Numerous papular lesions over the face |
 |
| Figure 1: Numerous papular lesions over the face |
Sir,
A 21-year-old old unmarried male presented to our Department with a 2 year history of numerous well-demarcated, firm, rubbery brownish yellow papular lesions of different sizes, over the face, neck, trunk and upper extremities, the majority being on the face. The patient was otherwise healthy. General examination of all vital systems was normal. Cutaneous examination revealed multiple skin-colored and hyperpigmented papules of different sizes, distributed over the face, neck, extensor and flexor aspects of the upper extremities [Figure - 1]. The trunk had a few lesions on the front and back. The lesions were asymptomatic, firm to rubbery in consistency and non-tender. Examination of mucous membranes, palms and soles was normal. The patient was a healthy active male, cycle mechanic by profession and denied any sexual contact of any type in the past. As per the patient′s version, lesions first started 2 years back on the face as a solitary papule over the right cheek, subsequently followed by appearance of multiple lesions in different parts as mentioned. A clinical diagnosis of late onset juvenile xanthogranuloma (JXG) was made and a biopsy was done. Histopathological examination revealed histiocytic proliferation with features of secondary ′xanthomization′ with the presence of foam cells, foreign-body giant cells and Touton giant cells, in the superficial dermis. The epidermis was thinned out and without any grenz zone. Lymphocytes, eosinophils and neutrophils were variably seen in the inflammatory infiltrate with absence of plasma cells. The histopathology confirmed the diagnosis of JXG. The patient was advised radiography of skull and chest, but results were non-contributory. Sonography of the abdomen and pelvis was also normal. Hematological and biochemical parameters including lipid profile were within normal limits. A peripheral smear examination ruled out any hematological malignancy. The patient was sent for an ophthalmologic checkup and fundoscopy but no abnormality was detected. Looking at the benign course of the disease and instances of spontaneous regression and absence of any specific therapy, the patient was discharged with counseling and advised to report for a regular yearly follow-up.
Helwig and Macknay first coined the term juvenile xanthogranuloma in 1954, [1] as a benign, asymptomatic and common self-healing disorder of non-Langerhans cell histiocytosis (LCH), affecting mostly infants, children and rarely adults. Eighty per cent cases appear in the first year of life [2],[3] and 20-30% cases present at birth. [2] There is no sexual or racial predilection. [4] Clinically, in 90% of JXGs, cutaneous lesions are solitary, with the head and neck being the most common sites of involvement. Extracutaneous sites involving the eye, lung, abdominal viscera and skull have been reported by many authors. Adult JXGs rarely regress spontaneously and reports of concomitant extracutaneous lesions are rare. [5]
Juvenile xanthogranuloma is the most common form of non-X histiocytosis. [6] It forms a heterogeneous group defined by the proliferation of cells with macrophage characteristics. It is important to recognize multiple adult xanthogranulomas, because of its good prognosis and the absence of visceral involvement, therefore requiring no investigations or aggressive treatments, a very important observation made by Punithwavathy et al., in their case report of adult onset xanthogranuloma. [7] Three main clinical forms are recognized: a small nodular/papular (2-5 mm); large nodular (5-20 mm); and giant xanthogranuloma (more than 20 mm). [8] But unusual clinical variants like mixed form, subcutaneous form, JXG en plaque have been reported recently. Multiple xanthogranulomas are extremely unusual in adults and that to occur in an eruptive manner is quite rare and three such cases have been associated with hematological malignancy (lymphocytic leukemia and monoclonal gammopathy). [8]
Clinical backgrounds of patients with adult-onset xanthogranuloma are somewhat different from those of patients with juvenile xanthogranuloma, but the histological findings of both forms of the disease are identical. Extracutaneous involvement of the eye orbit, lung, liver, testis, central nervous system, kidney etc. has been reported in childhood variants, but is not seen in the adult type. Though there has been established association of JXG with neurofibromatosis (NF-1) and juvenile chronic myelogenous leukemia (JCML) in the childhood type, this has never been reported in adults. Evaluation for extracutaneous JXG is not indicated, unless there are symptoms or findings suggesting their presence, as they also disappear spontaneously. Differential diagnosis includes molluscum contagiosum, cryptococcosis, benign cephalic histiocytosis (seen exclusively in children, infiltrate lacks foamy cells and multinucleated giant cells), generalized eruptive histiocytosis (absence of granulation and lipidation), xanthoma disseminatum (lesions tend to merge into plaques, mucous membrane involvement, associated diabetes insipidus and different biopsy findings), papular xanthoma (JXG histologically recognized by its pure primitive histiocytic phase and presence of inflammatory cells, not seen in papular xanthoma). The importance of presenting this case is to highlight the fact that while making a diagnosis of common disorders like molluscum contagiosum, one must keep in mind the adult form of xanthogranuloma in differential diagnosis.
| 1. |
Helwig EB, Macknay VC. Juvenile xanthogranuloma. Am J Pathol 1954;30:625.
[Google Scholar]
|
| 2. |
Giannoti F, Caputo R. Histiocytic syndromes: A review. Am Acad Dermatol 1985;13:383.
[Google Scholar]
|
| 3. |
Caputo R. Text Atlas of Histocytic Syndrome . London: Martin-Dunitz; 1988.
[Google Scholar]
|
| 4. |
Winkelmann RK. Cutaneous syndromes of non-X histiocytosis: A review of the macrophage histiocyte diseases of the skin. Arch Dermatol 1981;117:667-72.
[Google Scholar]
|
| 5. |
Shin SJ, Scamman W, Gopalan A, Rosen PP. Mammary presentation of adult-type "Juvenile" xanthogranuloma. Am J Surg Pathol 2005;29:827-31.
[Google Scholar]
|
| 6. |
Cohen BA, Hood A. Xanthogranuloma: Report on clinical and histologic finding in 64 patients. Pediatr Dermatol 1989;6:262-6.
[Google Scholar]
|
| 7. |
Punithwavathy K, Sentamilselvi G, Janaki VR, Janaki C. Late onset juvenile xanthogranuloma. Indian J Dermatol 1999;44:76-7.
[Google Scholar]
|
| 8. |
Caputo R, Grimalt R, Gelmetti C, Cottoni F. Unusual aspects of juvenile xanthogranuloma. J Am Acad Dermatol 1993;29:868-70.
[Google Scholar]
|
Fulltext Views
3,873
PDF downloads
2,373





