Translate this page into:
Paraneoplastic pemphigus associated with interdigitating dendritic cell sarcoma
-
Received: ,
Accepted: ,
How to cite this article: Jing J, Xu P, Lv ZF, Wu XJ. Paraneoplastic pemphigus associated with interdigitating dendritic cell sarcoma. Indian J Dermatol Venereol Leprol 2022;88:80-2.
Sir,
A 63-year-old woman presented with a five-month history of erosions on her lips and oral cavity, accompanied by a one-month history of itchy erythematous patches and blisters over the trunk and limbs. She was also severely malnourished. Five years ago, a large intra-abdominal mass was incidentally detected on ultrasound examination. On examination she had multiple ulcers and erosions with hemorrhagic crusts over her lips [Figure 1]. There was diffuse erythema, target lesions and blisters on her trunk and extremities. Nikolsky and bulla spread signs were negative [Figure 2]. Abdominal contrast-enhanced computed tomography revealed a 11.5 × 9 × 6.5 cm sized, densely enhancing soft tissue mass with necrosis in her left posterior lumbar and umbilical regions [Figure 3].
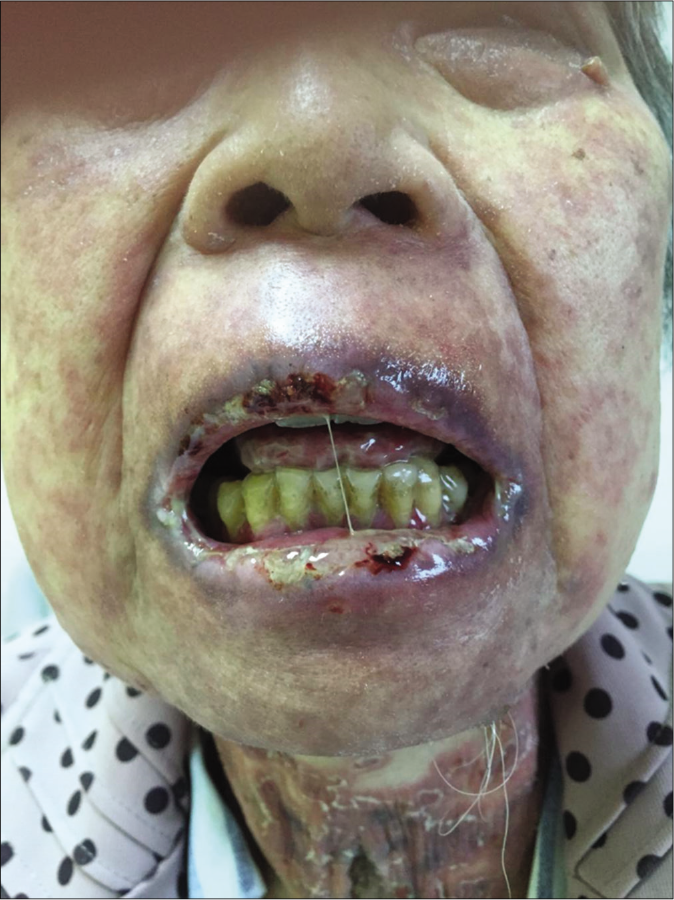
- Multiple erosions and hemorrhagic crusts over her lips
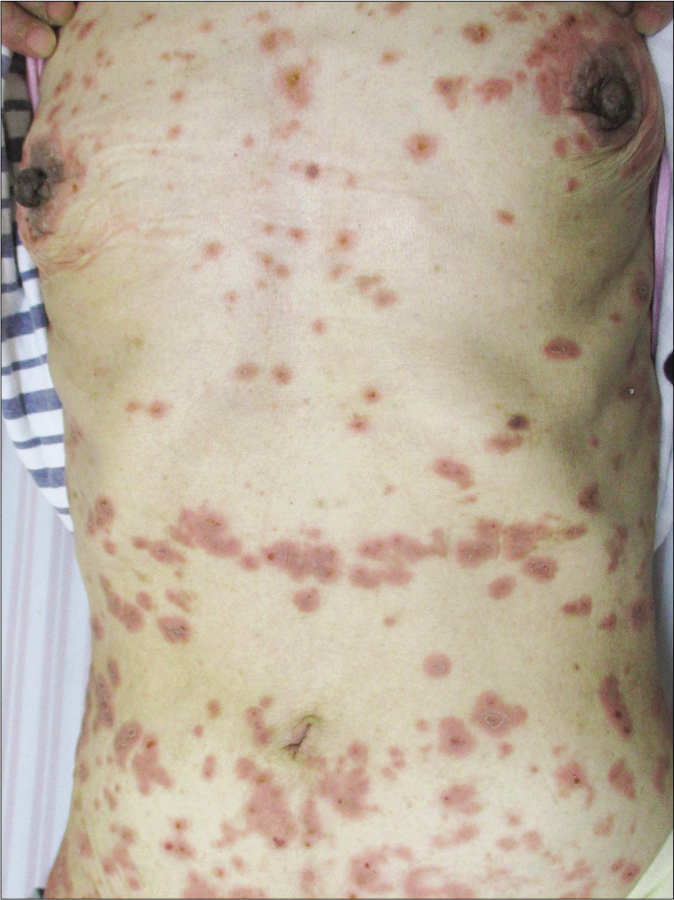
- Diffuse erythematous plaques, target lesions and blisters on the trunk
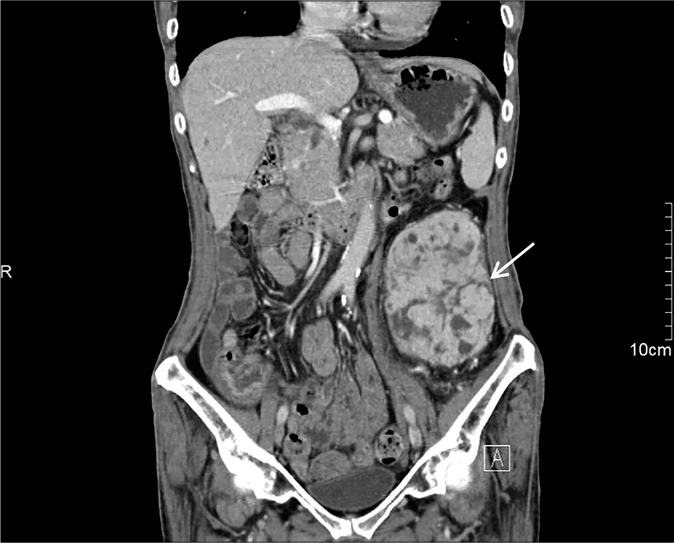
- Abdominal contrast-enhanced computed tomography revealed a 11.5 × 9 × 6.5 cm sized soft tissue mass with necrosis (white arrowhead)
Histopathologic findings from a skin biopsy taken from the skin on her left arm revealed acantholysis, intraepidermal blister and a dermal infiltrate of lymphocytes and eosinophils [Figure 4]. Direct immunofluorescence microscopy showed an intercellular deposition of IgG in the stratum spinosum [Figure 5]. An initial diagnosis of paraneoplastic pemphigus was made, and she was given intravenous methylprednisolone (40 mg/day) and intravenous immunoglobulin (20 g/day) for one week, but her lesions worsened.
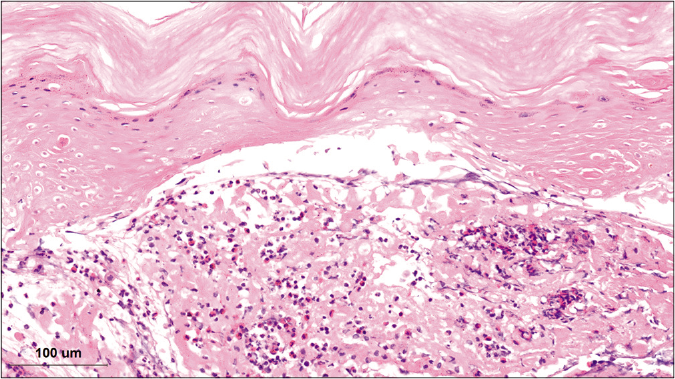
- Skin biopsy shows acantholysis, intraepidermalblister and infiltrate of lymphocytes and eosinophils (hematoxylin-eosin stain x500)
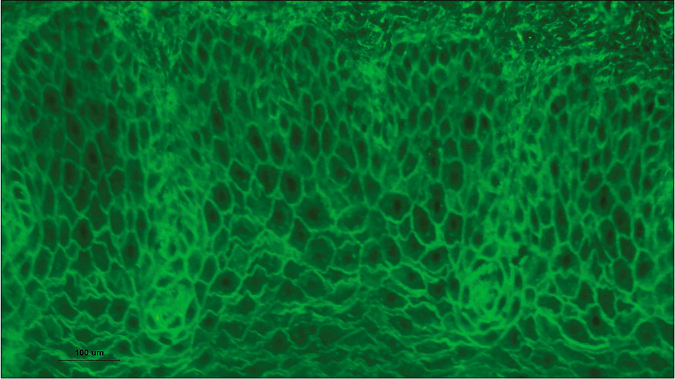
- Direct immunofluorescence revealed IgG deposition in the intercellular spaces in a reticular pattern (x500)
She subsequently underwent complete resection of the abdominal mass, which histologically revealed spindle-to-ovoid tumor cells arranged in a storiform pattern, intermingled with lymphocytes suggestive of a sarcoma [Figure 6]. On immunohistochemistry, the tumor cells were S-100- and CD68-positive and CD1a-negative, and the Ki67 index was 10%. The tumor cells also had scattered CD21-, CD23- and CD35-positivity and negative staining for clusterin and CXCL13. Based on these findings, a diagnosis of paraneoplastic pemphigus with interdigitating dendritic cell sarcoma was made. However, a week after surgical excision, the patient’s condition progressively deteriorated and she succumbed to multiple organ failure.
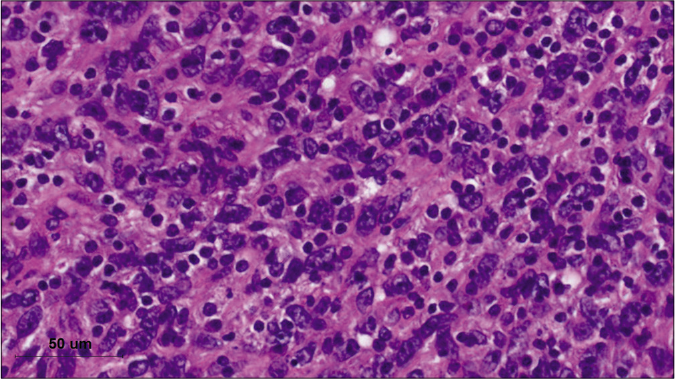
- Histologic findings of the mass reveal spindle-to-ovoid tumor cells forming in a whirlpool or storiform patterns, intermingled with dense lymphocytes (hematoxylin-eosin stain, x1000)
Paraneoplastic pemphigus is an autoimmune bullous disease characterized by severe stomatitis, polymorphous skin eruptions in the presence of an underlying neoplasm, most commonly Castleman’s disease, lymphoma or chronic lymphatic leukemia.1 Paraneoplastic pemphigus associated with interdigitating dendritic cell sarcoma is rarely reported. This tumor is an extremely rare malignancy derived from dendritic cells in lymphoid organs and predominantly affects the lymph nodes in middle-aged adults with one- third of cases showing extranodal involvement, such as the liver (27%), spleen (18%) and skin (15%).2 Clinically, the majority of patients present with disease in the head-and-neck region as a solitary mass. Histopathologically, the disease is characterized by neoplastic proliferation of spindle-shaped to ovoid cells arranged in nesting, fascicular or storiform patterns with numerous intermingled lymphocytes. The tumor cells are universally positive for S100, negative for CD21, CD23 and CD35 and variably positive for CD68. The main differential diagnosis is another rare dendritic cell neoplasm, follicular dendritic cell sarcoma which is negative for S100 but positive for a panel of follicular dendritic cell sarcoma markers including CD21, CD23, CD35, CXCL13 and clusterin.3-6 Young age, intra-abdominal involvement and combined nodal and extranodal involvement portend a poor prognosis in interdigitating dendritic cell sarcoma.3
Treatment of paraneoplastic pemphigus is aimed at treating the underlying neoplasm in an attempt to control the autoantibody response. However, paraneoplastic pemphigus and the underlying malignancy do not always have a parallel evolution. For interdigitating dendritic cell sarcoma, surgical excision followed by chemotherapy may be curative, but only in cases of localized tumor. Treatment of paraneoplastic pemphigus includes immunosuppressants on the same lines as pemphigus vulgaris.7,8 However, paraneoplastic pemphigus is usually more resistant to most treatments, including rituximab, than other pemphigus types and has a higher mortality.9 A more detailed analysis of the treatments for this disease in the future may be important for eliminating confusion regarding this subject.
Contributorship
In this manuscript, Jing Jing contributed to drafting of the article. Peng Xu contributed to the planning and collection of materials. Zhong-Fa Lv and Xian-Jie Wu contributed to revising and final approval of this article. Xian-Jie Wu was identified responsible for the article as the guarantor.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Clinical images: Castleman disease and paraneoplastic pemphigus. CMAJ. 2010;182:61.
- [CrossRef] [PubMed] [Google Scholar]
- A rare case of rectal interdigitating dentritic cell sarcoma presenting with a polypoid appearance. Pathology. 2016;48:744-6.
- [CrossRef] [PubMed] [Google Scholar]
- Impact of surgery, radiation and systemic therapy on the outcomes of patients with dendritic cell and histiocytic sarcomas. Eur J Cancer. 2015;51:2413-22.
- [CrossRef] [PubMed] [Google Scholar]
- Tumours of histiocytes and accessory dendritic cells: An immunohistochemical approach to classification from the International Lymphoma Study Group based on 61 cases. Histopathology. 2002;41:1-29.
- [CrossRef] [PubMed] [Google Scholar]
- Interdigitating dendritic cell sarcoma. J Natl Compr Canc Netw. 2015;13:128-32.
- [CrossRef] [PubMed] [Google Scholar]
- Identification of CXCL13 as a new marker for follicular dendritic cell sarcoma. J Pathol. 2008;216:356-64.
- [CrossRef] [PubMed] [Google Scholar]
- Polymorphic blistering eruption and stomatitis in a patient with non-Hodgkin lymphoma. JAMA Dermatol. 2015;151:439-40.
- [CrossRef] [PubMed] [Google Scholar]
- Paraneoplastic pemphigus: Insight into the autoimmune pathogenesis, clinical features and therapy. Int J Mol Sci. 2017;18:2532.
- [CrossRef] [PubMed] [Google Scholar]
- Paraneoplastic pemphigus: Paraneoplastic autoimmune disease of the skin and mucosa. Front Immunol. 2019;10:1259.
- [CrossRef] [PubMed] [Google Scholar]





